Diseases and Disorders of the Accessory Organs
April 11, 2024
Learning Objective: Examine the diseases and disorders of the accessory organs, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
A number of diseases and disorders affect the accessory organs: the salivary glands, liver, gallbladder, and pancreas. The following sections describe common diseases and disorders of the accessory organs.
Cholelithiasis
Learning Objective: Discuss cholelithiasis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Cholelithiasis (or gallstones) occurs when the substances in the bile harden and form stones (FIGURE 19.12). The stones can be small, like a piece of rice, or large, like a walnut. Cholesterol gallstones are the most common type and usually contain undissolved cholesterol. Pigment gallstones are darker black and occur when the bile contains too much bilirubin.
It is unclear why gallstones form, but it may be related to the bile containing too much cholesterol or bilirubin. They may also form if the gallbladder does not empty completely, causing the bile to become concentrated. Females, Native Americans, Mexican Americans, and people over age 40 are at higher risk for gallstones. Additional risk factors include the following:
• Eating a high-fat, high-cholesterol, or low-fiber diet
• Being overweight or obese; losing weight very quickly
• Having diabetes, leukemia, sickle cell anemia, or liver disease
• Having a family history of gallstones
• Taking estrogen-containing medication
If signs and symptoms are present, they may include nausea, vomiting, and referred pain. The person may have pain in the upper back, right shoulder, upper right abdomen, or below the sternum. Many of these symptoms are similar to a heart attack; thus they can be scary for the patient.

FIGURE 19.13 Endoscopic retrograde cholangiopancreatography (ERCP). From Frank ED, Long BW, Smith BJ: Merrill’s atlas of radiographic positions and radiologic procedures, ed 12, St. Louis, 2012, Mosby.
After a physical exam, a gallbladder radionuclide scan, MRI, or endoscopic retrograde cholangiopancreatography (ERCP) may be done. Treatment is based on the intensity of the symptoms. A cholecystectomy may be done. Gallstones can be removed during the ERCP (FIGURE 19.13). Patients who cannot undergo surgery may take medications to dissolve the gallstone, although it may take months or years to work.
19.8 Critical Thinking Application
Keith is rooming a female patient who works as an office assistant. She has had upper back and right shoulder pain, nausea, and vomiting for 2 days. The patient states that she has lost 50 pounds in the past 3 months. She is on oral contraceptives and acetaminophen for pain as needed. After examining the patient, Dr. Martin wants her to have an MRI for possible gallstones. What risk factors does this patient have for gallstones? What signs and symptoms does she have that are related to gallstones?
Cirrhosis
Learning Objective: Describe cirrhosis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Cirrhosis is a chronic liver disease. The liver cells are damaged and are replaced with scar tissue (FIGURE 19.14). The scar tissue reduces the liver’s ability to function, and over time the liver fails.
Diseases such as alcoholic liver disease, nonalcoholic fatty liver disease, and chronic hepatitis B and C cause cirrhosis. The signs and symptoms of cirrhosis may not appear until the liver is significantly damaged. Cirrhosis can cause nosebleeds, abdominal swelling, hypertension, kidney failure, jaundice, severe itching, gallstones, varices in the stomach and esophagus, and increased sensitivity to medications. Cirrhosis, like other liver diseases, can cause ascites, a buildup of fluid in the space between the organs and the abdominal lining.
Besides a medical history and physical exam, liver function tests, imaging tests, and a liver biopsy may be done. There is no cure for cirrhosis. Treatment of the underlying disease causing cirrhosis can help to slow liver destruction.
Hepatitis
Learning Objective: Describe hepatitis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Hepatitis is an inflammation of the liver. It can affect the functioning of the liver. Hepatitis can be an acute or chronic infection, depending on the type. There are different types of hepatitis, including alcoholic, toxic, autoimmune, and viral. With viral hepatitis, there are five main types of hepatitis: A, B, C, D, and E. In the United States, hepatitis A, B, and C are the most common. Vaccines to prevent hepatitis A and B are available.
Hepatitis is caused by alcohol use, toxins, certain medications and conditions, and viruses:
• Alcoholic hepatitis: Caused by heavy alcohol use.
• Toxic hepatitis: Caused by certain chemicals, medications, supplements, or poisons.
• Autoimmune hepatitis: A chronic type of hepatitis caused by the body’s immune system attacking the liver.
• Viral hepatitis: Hepatitis A virus (HAV) and hepatitis E virus (HEV) are spread from ingestion of food or drink contaminated by infected fecal matter. Hepatitis B virus (HBV), hepatitis C virus (HCV), and hepatitis D virus (HDV) are spread through contact with blood, semen, and other body fluids from an infected person. These viruses can also be passed from an infected mother to her baby during birth.
The signs and symptoms include fatigue, nausea, vomiting, anorexia, abdominal pain, clay-colored stools, dark urine, low-grade fever, joint pain, jaundice, and intense itching.
Besides a medical history and physical exam, the provider will order blood tests to diagnose hepatitis. Imaging tests may also be ordered. Screening for hepatitis C is recommended for adults ages 18 to 79. Treatment depends on the type of hepatitis. Chronic hepatitis may cause liver failure or liver cancer. A liver transplant may be needed. Treatment for hepatitis A and E includes bed rest and fluids. Supportive care is given with hepatitis D. Hepatitis B and C are treated with rest, interferon, and antiviral medications. Antiviral medications for hepatitis B include adefovir, entecavir, lamivudine, telbivudine, and tenofovir.
19.9 Critical Thinking Application
Summarize how hepatitis A, B, C, D, and E are transmitted. What strategies can be taken to prevent the transmission of each type?
Jaundice in the Newborn
Learning Objective: Discuss jaundice in newborns, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Jaundice in newborns can be life threatening. Jaundice is a condition caused by high levels of bilirubin in the blood. Bilirubin is a yellow to orange pigment that results when heme (from red blood cells) is broken down.
The cause of jaundice in newborns is hyperbilirubinemia (excess bilirubin). During the first days of life, red blood cells are produced and broken down at a faster rate compared to adults. In infants, the bilirubin can build up in the blood because the liver is not mature enough to get rid of it. Additional disorders that may cause jaundice in newborns include hemorrhage, infection, incompatibility between the mother’s blood and the baby’s blood, liver malfunction, red blood cell abnormality, and an enzyme deficiency. The risk for jaundice also increases with premature birth, significant bruising during birth, and breastfeeding. Signs and symptoms of jaundice include yellowish coloring of the skin and sclera, listlessness, poor feeding and weight loss, and high-pitched cries.
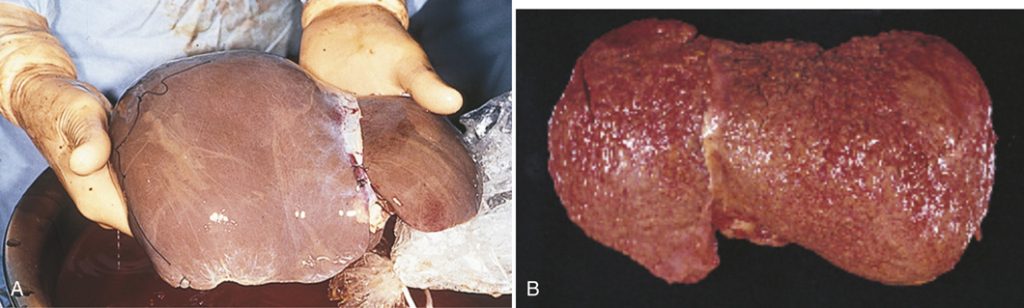
FIGURE 19.14 (A) Normal liver. (B) Cirrhosis of the liver. A, from Mahan LK, Escott-Stump S: Krause’s food and nutrition therapy, ed 12, Philadelphia, 2008, Saunders/Elsevier. B, from Damjanov I: Pathology: A color atlas, St. Louis, 2000, Mosby.
High levels of bilirubin can lead to severe complications in newborns. Acute bilirubin encephalopathy occurs when the bilirubin passes into the baby’s brain. Signs and symptoms include listlessness, difficulty waking, high-pitched crying, fever, backward arching of the neck and back, poor sucking, and poor feeding. Kernicterus occurs if acute encephalopathy causes permanent brain damage. Signs of kernicterus include involuntary and uncontrolled movements, a permanent upward gaze, and hearing loss.
The provider will do a physical exam and then order a blood test to measure the bilirubin level. Treatment may consist of these measures:
• Phototherapy: The infant is placed under a lamp that emits blue-green spectrum light, which changes the structure of the bilirubin molecule. The change allows the bilirubin to be excreted in the urine and stool. Light therapy can also be done using a light-emitting mattress or pad. The baby wears only a diaper and protective eye patches.
• Intravenous immunoglobulin (IVIg): Used for blood incompatibility–related jaundice. The immunoglobulin reduces the levels of antibodies and may reduce the jaundice.
• Exchange transfusion of blood: Used for severe jaundice.
Nonalcoholic Fatty Liver Disease
Learning Objective: Discuss nonalcoholic fatty liver disease, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Nonalcoholic fatty liver disease (NAFLD) causes a buildup of fat in the liver, unrelated to drinking alcohol.
The cause of NAFLD is unclear. The risks for NAFLD include obesity, prediabetes, type 2 diabetes, high cholesterol and triglycerides, and high blood pressure. Additional risks include rapid weight loss, gastric bypass surgery, bowel disease, and medications (e.g., calcium channel blockers and some chemotherapy drugs). A person with NAFLD may experience fatigue and upper right abdominal pain. If the person has liver damage, then weakness, loss of appetite, nausea, jaundice, itching, leg and abdominal swelling, GI bleeding, and mental confusion may be experienced.
Often NAFLD is found during routine blood tests. The provider may order additional laboratory tests, including a CBC, prothrombin time, and blood albumin level. US, MRI, a CT scan, and a liver biopsy may also be done. Treatment is focused on healthy choices, including losing weight, healthy eating, being physically active, and not drinking alcohol.
Pancreatitis
Learning Objective: Describe pancreatitis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Pancreatitis is an inflammation of the pancreas. The digestive enzymes start to break down the pancreas. If treated, acute pancreatitis may last a few days, but chronic pancreatitis worsens over time, and permanent damage occurs.
Gallstones commonly cause acute pancreatitis, and patients may have severe upper abdominal pain radiating to the back, a rapid pulse, nausea, and vomiting. Heavy alcohol use, cystic fibrosis, some inherited and autoimmune diseases, and certain medications can lead to chronic pancreatitis. Signs and symptoms of chronic pancreatitis include nausea, vomiting, weight loss, and oily stools.
Besides a medical history and physical exam, lab and imaging tests are used to diagnose pancreatitis. Treatment includes hospitalization, IV fluids, analgesics, antibiotics, and nutritional support (e.g., low-fat diet, enteral feeding).
Additional Diseases and Disorders of the Accessory Organs
Learning Objective: Describe additional diseases and disorders of the accessory organs.
The following diseases and disorders are related to the accessory organs.
• Acute cholecystitis: A sudden inflammation and swelling of the gallbladder, which causes severe abdominal pain; can be caused when a gallstone blocks the cystic duct, causing irritation and pressure in the gallbladder.
• Mumps: Caused by a viral infection, which leads to painful swelling of the salivary glands.
• Primary biliary cirrhosis: Chronic liver disease causing the bile ducts to be inflamed and damaged, leading to the buildup of bile in the liver.
• Hemochromatosis: Causes too much iron to build up in the body, especially in the liver, heart, and pancreas, which damages the organs and causes a bronze or gray skin color.
• Sialoliths: The buildup of crystallized saliva deposits blocks the flow of saliva, causing pain and swelling; also called salivary stones.
• Sialadenitis: A bacterial infection of a salivary gland, usually related to blockage of the duct; can cause a painful lump in the gland, severe pain, high fever, and foul-tasting pus in the mouth.
Gastrointestinal System Cancers
