Thyroid Gland and Parathyroid Gland Diseases and Disorders
April 11, 2024
Learning Objective: Examine thyroid gland and parathyroid gland diseases and disorders, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Hypersecretion and hyposecretion of the hormones from the thyroid and parathyroid glands cause diseases and disorders. The following sections examine thyroid and parathyroid diseases and disorders.
Thyroid Diseases
Learning Objective: Discuss hyperthyroidism and hypothyroidism, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Thyroid diseases cause hypersecretion or hyposecretion of thyroid hormone. TABLE 24.1 describes thyroid diseases. Hyperthyroidism and hypothyroidism are described in depth in the following sections.
Hyperthyroidism
Hyperthyroidism occurs when too much thyroid hormone is produced. Hyperthyroidism is more common in women, people with other thyroid conditions, and those over 60 years of age.
The most common cause of hyperthyroidism is Graves disease, and additional causes include thyroid nodules, pituitary disorders and tumors, and thyroiditis (see TABLE 24.1). Risk factors include a family history of thyroid disorders and having an existing autoimmune disease. Hyperthyroidism can cause the following conditions:
• Fatigue, muscle weakness, sensitivity to heat, and increased sweating
• More frequent bowel movements and weight loss, even with adequate food intake and an increased appetite
• Difficulty sleeping, restlessness, irritability, nervousness, and anxiety
• Rapid heart rate, irregular heart rate, and palpitations
• Goiter and exophthalmia (Figures 24.8 and 24.9)
• Changes in the menstrual cycle
• Thyrotoxicosis (thyroid storm), a life-threatening condition that causes elevated vital signs (e.g., temperature, pulse, respiration, and blood pressure)
Diseases That Cause Hyperthyroidism and Hypothyroidism
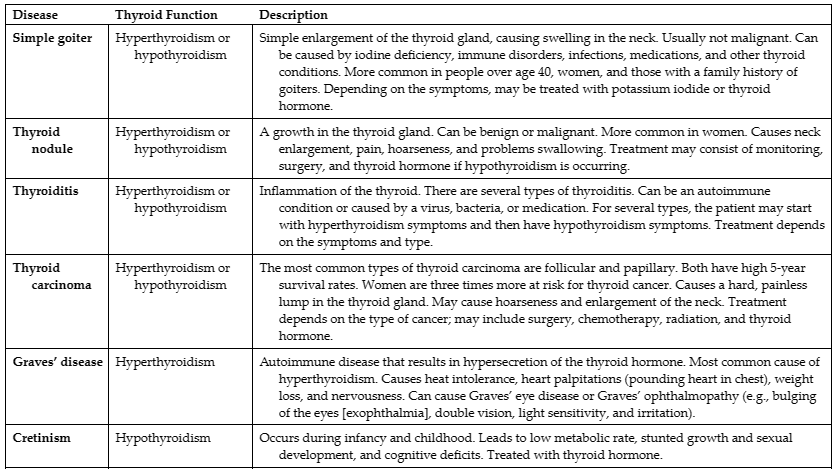


FIGURE 24.8 Goiter.
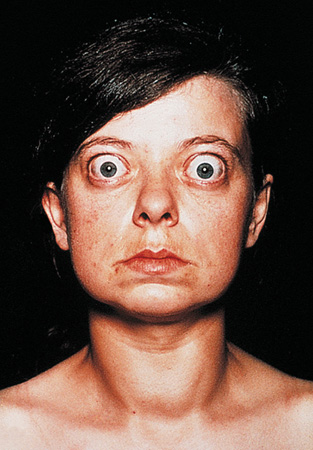
FIGURE 24.9 Exophthalmos in Graves’ disease
After performing a physical exam, the provider may order thyroid function tests and a radioactive iodine uptake (RAIU) scan. Treatment includes radioactive iodine therapy to shrink the thyroid, antithyroid medication (e.g., methimazole [Tapazole]), and a thyroidectomy.
Hypothyroidism
Hypothyroidism occurs when too little thyroid hormone is produced. Hypothyroidism occurs after thyroidectomy and radiation therapy. TABLE 24.1 describes additional conditions that cause hypothyroidism. Risk factors for hypothyroidism include having a history of an autoimmune disease, a family history of hypothyroidism, or pregnancy in the past 6 months. Another risk factor is being a female over 60 years of age. The signs and symptoms related to the metabolism slowing down and may include the following:
• Fatigue, muscle weakness, tenderness, aches, and stiffness
• Constipation and weight gain
• Dry skin, sensitivity to cold, and thinning hair
• Slowed heart rate, hoarseness, and depression
• Elevated blood cholesterol
After the provider performs the physical exam, thyroid function tests and a thyroid ultrasound may be done. Treatment requires taking lifelong synthetic thyroid hormone (e.g., levothyroxine [Synthroid]).
24.4 Critical Thinking Application
Cecilia is working with a patient who has been diagnosed with hypothyroidism. What are the signs and symptoms of hypothyroidism? What treatments are usually prescribed?
Parathyroid Gland Diseases
Learning Objective: Discuss hyperparathyroidism and hypoparathyroidism, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Hyperparathyroidism occurs when there is hypersecretion of parathyroid hormone, and hypoparathyroidism occurs when there is hyposecretion of the hormone.
Hyperparathyroidism
Hyperparathyroidism is a relatively common disorder. It occurs when one or more of the four parathyroid glands oversecrete PTH. Hyperparathyroidism causes excessive bone resorption, and the calcium from the bones causes hypercalcemia (abnormally high blood calcium level).
Primary hyperparathyroidism occurs as a result of an adenoma or hyperplasia of one of the four glands, causing an increase in PTH secretion. Secondary hyperparathyroidism occurs with renal disease, which causes hypocalcemia and low vitamin D levels that trigger PTH secretion. The signs and symptoms are related to hypercalcemia and include the following:
• Muscle pain, atrophy, and weakness
• Gastrointestinal pain, nausea, vomiting, and anorexia
• Cardiac arrhythmias, renal calculi, bone tenderness, and fractures
After the physical exam, the provider may order blood tests (e.g., calcium, phosphorus) and imaging tests (e.g., x-ray studies, bone density tests, radioimmunoassay studies). Treatment depends on the cause. Minimally invasive surgery may be done to remove a tumor or gland(s). When hyperplasia occurs, all but half of a gland can be removed. For secondary hyperparathyroidism, the underlying cause is treated. Medications may be prescribed to help increase calcium excretion by the kidneys.
24.5 Critical Thinking Application
Cecilia is rooming Mr. Jones, who came with his wife, Sally. Over the past few months, he has been depressed, forgetful, and weak. At times he has experienced abdominal pain and joint pain. His primary care provider diagnosed him with hyperparathyroidism, and today he came to see the specialist. Mr. Jones had never heard about the parathyroid gland, and he asked Cecilia about it. How would you explain the parathyroid gland to a patient?
Hypoparathyroidism
Hypoparathyroidism occurs when there is hyposecretion of parathyroid hormone. This reduction of PTH causes hypocalcemia to occur.
Hypoparathyroidism results from injury or damage to the parathyroid glands. Damage and destruction of the glands can result from cancer, radiation, and surgery (e.g., thyroidectomy). The signs and symptoms relate to the hypocalcemia and can include the following:
• Numbness and tingling, spasms, and twitching in the hands and feet
• Confusion and irritability
• Tetany (continuous muscle spasms), laryngospasm, arrhythmias, respiratory paralysis, and death
The provider will perform a physical exam and order blood tests (e.g., calcium, phosphate), an electrocardiogram, and imaging tests (e.g., radioimmunoassay studies). Lifelong treatment includes calcium and vitamin D supplements and a high-calcium diet.
