Elimination
June 23, 2023
Gastrointestinal System
Slowing of intestinal peristalsis can result in abdominal distention, flatulence, and constipation. Constipation may also be linked to iron supplements the woman is taking.
Hemorrhoids can result from straining as a result of constipation. They can also be caused by the enlarged uterus putting pressure on the pelvic blood vessels, slowing venous return from the lower extremities. Women with a history of cholelithiasis may experience problems with this as a result of an increased cholesterol level, which is common during pregnancy. Adequate fluid intake, dietary roughage, and exercise may help reduce problems related to constipation.
Urinary System
Frequency of urination is a common symptom of pregnancy. In the first trimester, this results from the enlarging uterus putting pressure on the bladder. Later, during the third trimester, the uterus moves back into the pelvic cavity in preparation for labor and delivery, again placing pressure on the urinary bladder. The increase in circulating blood volume results in increases in glomerular filtration rates (GFR). This causes an increase in urinary output. The stressors placed on the kidneys during pregnancy may result in protein and glucose to be detected in the urine samples. During the prenatal care period, the woman’s urine is evaluated with a dipstick test to assess for the presence of glucose or protein. The patient can be taught Kegel exercises to help tone the muscles of the perineum and prevent stress incontinence (see Patient Teaching box on Kegel exercises).
The ureter and kidneys may become dilated, particularly on the right side, as a result of placental progesterone and pressure from the enlarging uterus. Restricted circulation in the pelvis as the uterus enlarges increases the risk of bladder trauma and urinary tract infection.
Activity and Exercise
Patients should continue normal activity throughout an uncomplicated pregnancy. If a woman regularly participates in a fitness program or sport, she probably can continue with most activities. This should be discussed with the health care provider. High-risk activities or those that require a great deal of balance and coordination are discouraged. Common sense is the best guide.
Changes in balance and posture occur as the fetus increases in size. To compensate for the shifting center of gravity, the lumbodorsal curve increases (lordosis), which may result in low backaches. Hormonal influence on pelvic bones, which results in joint relaxation, can lead to a waddling gait. Footwear with low heels and the use of good body mechanics help reduce discomfort.
Leg cramps are common, perhaps related to pressure on the pelvic blood vessels and nerves or altered calcium and phosphorus balance. Dorsiflexion of the
Patient Teaching: Kegel Exercises
- • The muscles that stop the flow of urine are the pubococcygeal muscles. These muscles support the pelvic floor, the bladder, and the urethra. Attempts to stop the flow of urine or forestall the expulsion of gas aid the woman in targeting the involved muscles. Doing Kegel exercises during urination helps the woman know whether she is doing them correctly. If she can stop the stream of urine, her tone is good.
- • After a woman has located the targeted muscles, she can do Kegel exercises in the following ways:
- • Slow: Tighten the muscle, hold it for a count of 3, and relax it.
- • Quick: Tighten the muscle, and relax it as rapidly as possible.
- • Push out, pull in: Pull up the entire pelvic floor as though trying to suck up water into the vagina. Then, bear down as if trying to push the imaginary water out. This also uses abdominal muscles.
Practice
- • Kegel exercises must be practiced several times a day to be effective. They must be done every day for the rest of the woman’s life.
- • These exercises can be done 10 times in a row at least 3 times or more per day. Although some people recommend doing this as many as 100 times in a row, this only fatigues the pelvic floor muscles.
- • A good time to practice is during trips to the bathroom, but additional practice at other times is even more beneficial.
Fatigue is common reported during pregnancy. The woman must pace herself and not overdo tiring activities.
foot may help reduce these cramps. Dependent edema and varicose veins can also result from increasing intraabdominal pressure. Many women wear support hose to reduce edema; resting with legs elevated is also helpful.
Round ligament pain or tenderness in the lower abdomen is a result of stretching of the ligaments by the enlarging uterus. There is no way to prevent this, but use of good body mechanics reduces the discomfort.
Dyspnea (shortness of breath) may be experienced as the uterus enlarges and pushes the diaphragm upward, decreasing the size of the chest cavity. Avoiding large meals, which distend the stomach, and maintaining good posture help relieve this problem. Exercises are often recommended to help reduce discomfort and prepare for childbirth (Box 25-11).
Rest and Sleep
Early in pregnancy, women experience increased fatigue. Napping is encouraged during this time. Left side–lying positioning is recommended to promote oxygenation. As the pregnancy progresses and the
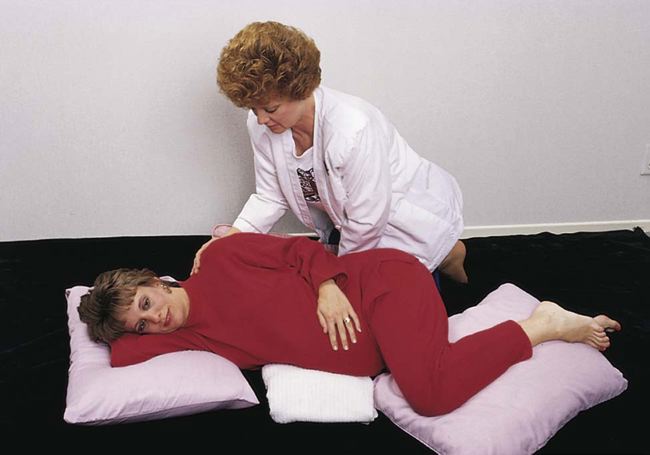
abdomen grows larger, the pregnant woman may have difficulty finding a position of comfort, particularly if she prefers to sleep in the prone position. The supine position is not recommended because the enlarged uterus may place excessive pressure on the aorta and vena cava. The pressure can result in vena cava syndrome (supine hypotensive syndrome). The woman may experience syncope and vertigo. The supine position also may result in decreased circulation for the fetus. A side-lying position is recommended (Figure 25-7).
Encourage rest periods during the day with feet elevated. Placing pillows under the legs and abdomen promotes good body alignment and rest. Naps at intervals during the day can be helpful, but these are not always possible with busy lifestyles.