Initiating IV Infusions
April 11, 2024
Initiating IV Infusions
Learning Objective: Demonstrate how to initiate an IV infusion, including priming the infusion set, preparing the site, and inserting the IV catheter.
When a medical assistant must initiate an IV infusion, preparation must be done before inserting the IV catheter. The medical assistant must prime the primary infusion set and prepare the site for the catheter insertion. After the catheter insertion, the medical assistant must document the procedure. The following sections discuss these procedures.
Priming the Primary Infusion Set
Learning Objective: Describe how to prime the primary infusion set.
The preparation begins with an order from the provider. The order must include the following:
• Patient’s name and date of birth (DOB)
• Type of IV solution
• Amount of fluid to infuse over a specific time period (e.g., 500 mL over 4 hours) or the rate of the infusion for a specific time period (e.g., 125 mL/hr × 4 hours)
As described earlier, IV orders may vary. The medical assistant must follow the nine rights of medication administration described in Chapter 15. The IV label must be compared to the order three times prior to the start of the infusion. The expiration date on the bag of fluid must also be checked.
The primary infusion set must be primed with the IV solution just before it is used. Priming means running IV fluid through the tubing to remove all of the air. This procedure prevents air from entering the patient’s circulatory system, which can cause an air embolism. Deaths have been attributed to as little as 10 mL of air. Procedure 36.1 describes how to prime the infusion set.

FIGURE 36.7 Common IV sites in adults. (A) Inner arm. (B) Dorsal surface of hand. From Potter PA, Perry AG: Fundamentals of nursing, ed 9, St. Louis, 2017, Elsevier.
As the medical assistant prepares the IV supplies, it is important to use sterile technique. The sterile spike, which is used to spike the IV bag, must remain sterile. The luer connector, found on the opposite side of the infusion set, also must remain sterile.
Identifying a Vein
Learning Objective: Discuss how to identify a vein for an IV catheter insertion.
In ambulatory care, a peripheral IV is usually inserted in an upper extremity. When looking for a potential insertion site, the medical assistant should start distally and work up the hand and arm (FIGURE 36.7). If an IV attempt is unsuccessful, all future sites must be more proximal to that site. In other words, the medical assistant should start looking for a vein on the top of the hand and move up the arm. If a site on the arm is unsuccessful, the medical assistant cannot attempt a site more distal, such as on the hand. The IV catheter should not be inserted in the following locations:
• In an area that is painful, tender, infected, burned, or compromised (e.g., lymphedema)
• In an area with an open wound
• In an extremity that is paralyzed or affected by a stroke, contains a dialysis fistula, or on the same side of a mastectomy
• Distal to a previous IV site or infiltrated site
• In a fragile vein
The medical assistant should avoid inserting the catheter in areas of flexion. Inserting the catheter in the antecubital site, on the inside of the wrist (ventral surface), or in the cephalic vein at the wrist can increase the risk for nerve damage.
Typically, the IV catheter is inserted and removed during the same visit. If the patient needs the IV catheter to remain in for a longer period of time, the medical assistant must consider the following:
• If possible, use the nondominant hand/arm.
• Avoid inserting the catheter in the hand if the patient is using an assistive device, such as a walker or cane.
• Avoid inserting the catheter in a flexible area, such as near the wrist or elbow.
The medical assistant should look for a straight, nonbranched vein (Procedure 36.2). The tourniquet can be placed about 4 to 6 inches proximal to the site to help the vein engorge with blood (FIGURE 36.8). When using the tourniquet, the medical assistant must check the patient’s radial pulse on the side with the tourniquet. If the radial pulse is diminished or absent, loosen the tourniquet. Here are some other strategies to help engorge the vein:
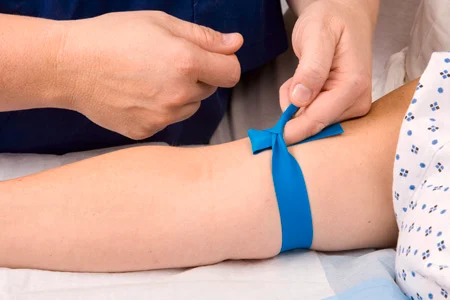
FIGURE 36.8 Tourniquet placed on arm for initial vein selection. From Potter P, Perry A: Basic nursing, ed 7, St. Louis, 2011, Mosby.
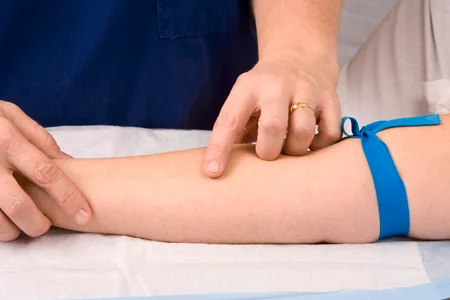
FIGURE 36.9 Palpate vein. From Potter P, Perry A: Basic nursing, ed 7, St. Louis, 2011, Mosby.
• Stroking the vessel
• Have the patient dangle their arm down on the side
• Applying a warm pack to the site for a few minutes
• Having the patient open and close the hand, making a fist
When the medical assistant palpates the vein, it should feel spongy (FIGURE 36.9). If the vessel is pulsing, it is likely to be an artery and should not be used. Some facilities use technology to help find a vein for catheter placement. Visible light devices transilluminate the vessel, and near infrared and ultrasound can also be used. Once the insertion site is determined, the tourniquet is removed.
Site Preparation
Learning Objective: Describe how to prepare the site for an IV catheter insertion.
If the patient’s skin is visibly soiled, it should be washed with soap and water and dried. If hair needs to be removed from the site, a disposable-head electric shaver can be used. Shaving is usually done for IVs that will remain in for a long period of time.
The skin can be cleaned using several different antiseptics. Always check the patient’s allergies before starting the procedure. The most common antiseptics include chlorhexidine, povidone-iodine (Betadine), and alcohol. Chlorhexidine is the preferred antiseptic. When using chlorhexidine, place the applicator on the skin and do a friction scrub (FIGURE 36.10). Scrub back and forth and up and down for 30 seconds. Allow the product to dry on the skin for at least 30 seconds. If using Betadine or alcohol, place the applicator at the intended site of insertion and work outward in a circular pattern, making larger circles as the area is cleaned. Betadine must dry before starting the catheter insertion. The drying process kills the microorganisms. If the skin is touched with gloves or ungloved hands, the cleansing process needs to be repeated.
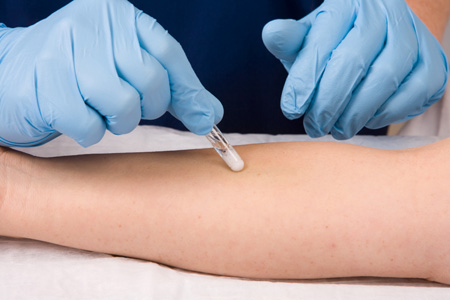
FIGURE 36.10 Cleanse site with chlorhexidine. From Potter PA, Perry AG: Fundamentals of nursing, ed 9, St. Louis, 2017, Elsevier.
36.5
Critical Thinking Application
A patient asks you why you need to clean the arm for so long before putting in the IV. How would you respond to this question?
Inserting the IV Catheter
Learning Objective: Describe how to insert an IV catheter.
Once the antiseptic is dried, the tourniquet is reapplied. Using the dominant hand, grasp the IV needle/catheter unit and place it parallel to the vein. Using the nondominant hand, hold the skin taut below the insertion site. The thumb should stabilize the vein in place during the insertion process.
With the bevel facing up, insert the needle/catheter unit directly on top of the vein using a 10- to 30-degree angle. Superficial veins require a lesser angle of insertion, whereas a deeper vein requires a greater angle. Once the needle enters the vein, a blood flashback is seen in the clear flashback chamber. The needle should be advanced a bit further. Then the catheter is pushed off the needle and advanced into the vein until the hub reaches the insertion site. A blood flashback may also be seen in the catheter as the catheter enters the vein. The needle is withdrawn, and the tubing is attached to the catheter. The catheter is taped to the arm, and a transparent or gauze dressing is applied. The infusion set is also secured to the arm with tape. After the IV catheter is inserted and the solution is infusing, the medical assistant should observe the site for a few minutes to ensure no complications occur.
If the patient experiences tingling or numbness during the insertion process or the infusion, the medical assistant should pause the infusion and notify the provider. This type of pain can indicate nerve damage.
If the medical assistant is unsuccessful with the insertion attempt, the entire cleansing process must be repeated in another location proximal to the attempted site. A new catheter must be used. The standard is two insertion attempts per person, with a total of four attempts.
36.6
Critical Thinking Application
When inserting an IV, Gabe warns the patient, “You will feel a poke,” just before he inserts the IV. Is this a good practice? Why or why not?
Documentation
Learning Objective: Describe the documentation required for an IV insertion.
After completing the catheter insertion and starting the IV infusion, the medical assistant must document the procedure. The documentation should include the following information:
• Date and time
• Ordering provider’s name
• IV order, which includes the IV solution, amount, and rate per hour or over the number of hours
• Type and size of catheter inserted
• Location of insertion site
• Any issues with the insertion process, including the number of insertion attempts
• Type of IV fluid being infused and the infusion rate
• Name and credentials (e.g., registered medical assistant [RMA]) of the person who inserted the catheter
• Any other documentation required by the facility
