Intestinal Diseases and Disorders
April 11, 2024
Learning Objective: Examine the diseases and disorders of the intestines, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Many intestinal diseases and disorders occur in adults, but some conditions affect children. The following sections describe common diseases and disorders of the intestine.
Acute Appendicitis
Learning Objective: Describe acute appendicitis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Appendicitis is an inflammation of the appendix. Commonly, it occurs between the ages of 10 and 30, though it can occur at any age.
The etiology is a blockage in the appendix that can increase pressure, affect blood flow, and cause inflammation. If the blockage is not treated, the appendix can burst and cause peritonitis (inflammation of the peritoneum), a life-threatening condition. The pain usually begins near the umbilicus and then moves to the lower right side of the abdomen. Rebound pain can occur with peritonitis. Additional signs and symptoms include low fever, abdominal bloating, anorexia, nausea, vomiting, constipation, diarrhea, and an inability to pass gas.
After the physical exam, blood and urine laboratory tests will be performed to rule out other conditions. A complete blood count (CBC) will show an elevated white blood cell count. Imaging tests (e.g., x-ray, computed tomography [CT] scan, and abdominal ultrasound [US]) will be done to confirm appendicitis or rule out other conditions. Treatments consist of antibiotics and an appendectomy. Laparoscopic surgery will result in a few small incisions. If a laparotomy is done, the incision may be 2 to 4 inches long. If the appendix bursts and an abscess forms, surgery may be delayed while the abscess is drained.
Celiac Disease
Learning Objective: Discuss celiac disease, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Celiac disease, also called gluten-sensitive enteropathy or celiac sprue, is a digestive and autoimmune disorder. When people with this disease eat foods with gluten, their immune system damages their small intestine. Gluten, a protein, is found in barley, rye, wheat, spelt, and triticale. It can also be found in other products, including vitamins and supplements, toothpaste, lip balm, and hair and skin products.
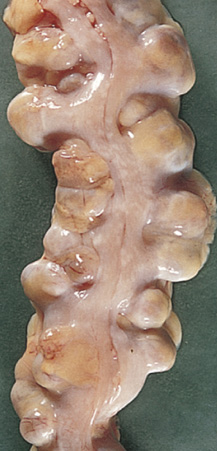
FIGURE 19.8 Diverticulitis. From Damjanov I: Pathology: a color atlas, St. Louis, 2000, Mosby.
Celiac disease is a genetic autoimmune disorder. The signs and symptoms of celiac disease can vary depending on the age of the person:
• Young children: Abdominal pain, vomiting, diarrhea, bloating, and constipation; irritability, emotional withdrawal, or very dependent behavior; failure to gain weight and grow; and obesity.
• Teenagers: Diarrhea, constipation, delayed puberty, hair loss, slowed growth, and short height.
• Adults: Diarrhea, constipation, fatigue, bone or joint pain, depression, anxiety, irritability, missed menstrual periods, anemia, and osteoporosis.
• Celiac disease can also cause lactose intolerance, anemia, dermatitis herpetiformis (an itchy, blistering skin condition), and canker sores in the mouth.
The provider will perform a history and physical exam. Blood tests and an intestinal biopsy may be ordered. Treatment consists of a gluten-free diet. Foods that are safe to eat include rice, oats, corn, quinoa, millet, and buckwheat.
Diverticulitis
Learning Objective: Describe diverticulitis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Diverticula are small marble-sized pouches that form in the large intestine (FIGURE 19.8). The pouches protrude through the weakened walls of the large intestine. These pouches are common after age 40 and usually do not cause symptoms unless they become inflamed or infected. When the diverticula become inflamed or infected, the condition is called diverticulitis.
When a diverticulum tears, inflammation and infection can occur. Risk factors include aging, obesity, smoking cigarettes, lack of exercise, a low-fiber diet, and a high saturated fat diet. Medications such as steroids, opioids, and NSAIDs can also increase the risk. Signs and symptoms of diverticulitis include constant lower left abdomen pain and tenderness, nausea, vomiting, diarrhea, constipation, and fever.
After a physical exam, the provider will order imaging and medical laboratory tests. Blood and urine tests are used to rule out infection, pregnancy, and liver disease. A CT scan can identify the inflamed pouches, thus confirming the diagnosis. Treatment depends on the symptoms. Antibiotics, over-the-counter (OTC) analgesics, and a liquid diet may be recommended. With severe attacks, intravenous (IV) antibiotics are given, and abscesses, if present, are drained. A primary bowel resection or a bowel resection with a colostomy may be done.
Foodborne Illnesses
Learning Objective: Describe diverticulitis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Eating or drinking contaminated food can result in a food-borne illness. Typically, food-borne diseases and disorders are acute illnesses, which occur suddenly and last for a short time. Most people recover without treatments, though sometimes more serious complications can occur.
Many different types of bacteria, viruses, parasites, and chemicals can contaminate food:
• Salmonella: Found in raw or undercooked meat, poultry, and seafood. It can also be found in dairy products, eggshells, and inside eggs.
• Shigella: Bacterium that spreads to others from one infected person’s unwashed hands after using the bathroom.
• Escherichia coli (E. coli): Found in raw or undercooked hamburger, unpasteurized milk and fruit juices, and fresh produce.
• Listeria monocytogenes: Found in raw and undercooked meats, unpasteurized milk, deli meats, soft cheeses, and hot dogs.
• Clostridium botulinum: Found in improperly canned foods and smoked and salted fish.
• Norovirus: Found in foods prepared by infectious food handlers; can cause inflammation of the intestines and stomach.
• Hepatitis A: A virus spread through food or drinks contaminated with a small amount of stool from an infected person.
• Trichinella spiralis: A roundworm parasite found in raw or undercooked pork or wild game.
Common signs and symptoms include vomiting, diarrhea, abdominal pain, chills, and fever. Symptoms may last for a few hours to a few days. Complications can lead to dehydration, hemolytic uremic syndrome, and other disorders, such as reactive arthritis and irritable bowel syndrome.
After a physical exam, the provider may order a stool culture and blood work. Treatment consists of replacing lost fluids and electrolytes. Over-the-counter antidiarrheal medications such as loperamide (Imodium) and bismuth subsalicylate (Pepto-Bismol, Kaopectate) can help decrease diarrhea in adults. These medications should not be used if the person has bloody diarrhea, which could be a sign of a parasitic or bacterial infection.
Hemorrhoids
Learning Objective: Describe hemorrhoids, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Hemorrhoids are swollen and inflamed veins. External hemorrhoids are located around the anus, and internal hemorrhoids affect the lining of the anus and the lower rectum. About 50% of those over 50 years of age have hemorrhoids.
Hemorrhoids can be caused by straining during a bowel movement, pregnancy, aging, chronic constipation, and diarrhea. The most common symptom of internal hemorrhoids is bright red bleeding, which usually goes away within a few days. Anal itching can occur with external hemorrhoids.
During the physical exam, the provider will check the anal area and perform a digital rectal exam. An anoscope, a proctoscope, or a sigmoidoscope may be used to examine the lower part of the large intestine and rectum. Home treatment includes a high-fiber diet, topical treatments (e.g., hydrocortisone, analgesic), sitz baths (soaking in a warm bath), cold packs, oral analgesics, and keeping the area clean.
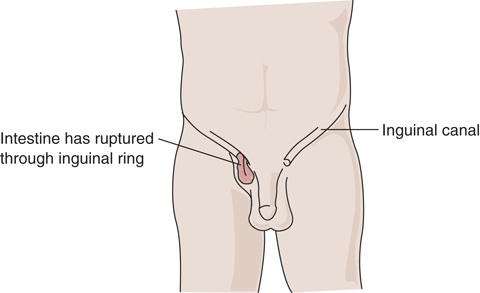
FIGURE 19.9 Inguinal hernia.
Hernia
Learning Objective: Describe hernias, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
A hernia is a common disorder that occurs when part of an internal organ (e.g., intestine) bulges through a weak area in the muscles. The hiatal hernia was already discussed in a prior section. Other types include the following:
• Femoral hernia: A bulge below the groin, in the upper thigh. More common in women.
• Inguinal hernia: Most common type of hernia. A bulge forms in the groin and may extend into the scrotum.
• Umbilical hernia: The muscle around the umbilicus does not close at birth, and a bulge forms.
Inguinal Hernia
An inguinal hernia occurs when tissue (e.g., part of the intestine) protrudes through a weak spot in the abdominal muscles (FIGURE 19.9). Sometimes people can gently push the hernia back into the abdomen, but other times the hernia may become trapped (incarcerated), and blood flow may be cut off to the tissue (strangulation), causing tissue death. This can be a life-threatening complication if it is not treated.
For some inguinal hernias, the etiology is unknown. Other times, straining, strenuous activities, pregnancy, or chronic coughing may cause it. Signs and symptoms include bulging on the side of the pubic bone, burning or aching at the bulge, and groin heaviness, pain, or pressure.
The provider will do a physical examination. The patient may be asked to stand and cough, which makes the inguinal hernia more prominent. A CT or magnetic resonance imaging (MRI) scan may be ordered if the hernia is not felt. For a small hernia that is asymptomatic, the provider may just wait and monitor it. Painful or enlarged hernias are treated with surgery (either an open hernia repair or a laparoscopic repair).
Inflammatory Bowel Disease
Learning Objective: Discuss inflammatory bowel disease, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Inflammatory bowel disease (IBD), an autoimmune disorder, includes two chronic diseases that cause inflammation of the digestive tract:
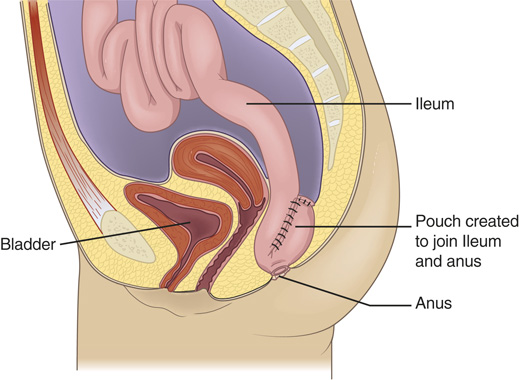
FIGURE 19.10 Ileal pouch–anal anastomosis (IPAA).
• Ulcerative colitis: Usually starts in the rectum and spreads into the large intestine. Damaged areas are in patches along the intestine. The inflammation may affect many layers of the GI tract wall.
• Crohn disease: Can affect any part of the GI tract but most often affects the ileum. Damage appears in patches next to healthy tissue. The inflammation affects several layers of the GI tract walls.
The etiology of IBD is unknown, but it is the result of a defective immune system. IBD has a genetic component, and environmental triggers cause inflammation of the digestive tract. Common signs and symptoms of IBD include persistent diarrhea, abdominal pain, blood in the stool, weight loss, and fatigue.
After the medical history and physical exam, the provider will order imaging tests and endoscopy exams. Stool samples are tested to rule out other conditions. Treatment consists of corticosteroids, immunomodulators, and biologics. Severe IBD may require surgery to remove the damaged GI tract. Common surgical procedures include colectomy, proctocolectomy, proctocolectomy with ileal pouch-anal anastomosis (IPAA), and ileostomy (FIGURE 19.10).
Intestinal Obstructions
Learning Objective: Discuss intestinal obstructions, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Intestinal obstructions are also called bowel obstructions. The obstruction can be either partial or complete and prevents stool or food from moving through the intestine. A complete intestinal obstruction is a medical emergency.
The obstruction can be related to a mechanical cause, such as adhesions, hernias, volvulus, impacted feces, and cancers. A nonmechanical obstruction, also called ileus or paralytic ileus, occurs because peristalsis stops. A paralytic ileus can be caused by infections, certain medications (e.g., narcotics), an electrolyte imbalance, a decrease in intestinal blood flow, or abdominal surgery. Signs and symptoms include severe abdominal pain, cramping, bloating, nausea, vomiting, swelling of the abdomen, loud bowel sounds, inability to pass flatus (gas), and constipation.
Tests to diagnose an intestinal obstruction can include an abdominal CT scan, an abdominal x-ray, a lower gastrointestinal (LGI) series, and an upper gastrointestinal (UGI) series. Treatment includes hospitalization and a nasogastric tube (a tube passed from the nose to the stomach), which is used to relieve abdominal contents and swelling. A bowel resection surgery may be required if the obstruction continues. A temporary or permanent colostomy may be done (FIGURE 19.11).
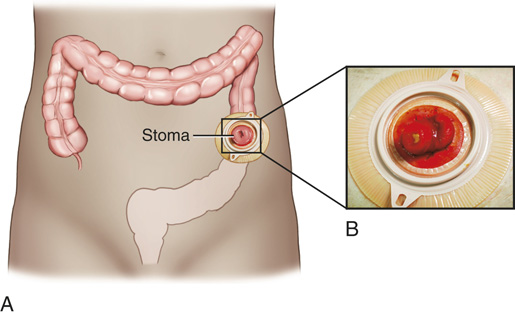
FIGURE 19.11 (A) Colostomy. (B) The inset shows the stoma. Potter PA, Perry AG: Fundamentals of nursing, ed 7, St. Louis, 2011, Mosby.
Irritable Bowel Syndrome
Learning Objective: Discuss irritable bowel syndrome, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Irritable bowel syndrome (IBS) is a disorder of the large intestine, although it does not cause harm to the colon. IBS is a common disorder, affecting females twice as often as males. People younger than age 45 often have IBS.
There is no known cause of IBS. Factors that may lead to IBS include changes in peristalsis, severe infection, early life stress, and changes in the intestinal microbes. Stress can increase the symptoms of IBS. The signs and symptoms include abdominal cramping, bloating, constipation, and diarrhea. Sometimes people go back and forth between diarrhea and constipation.
There is no specific test for IBS. The provider may do a colonoscopy, an upper endoscopy, x-ray, or CT scan to rule out other diseases. Treatment for IBS includes dietary changes, stress management, medications, and probiotics.
Additional Intestinal Diseases and Disorders
Learning Objective: Describe additional intestinal diseases and disorders.
The following list presents additional intestinal diseases and disorders:
• Anal fissure: A small tear (fissure) in the anal mucosa that causes pain.
• Anorectal abscess: A collection of pus in the anal and rectal area caused by a blocked gland, an anal fissure, trauma, or a sexually transmitted infection (STI). Deep rectal abscesses can be caused by intestinal disorders such as Crohn disease.
• Bowel incontinence: Accidental passage of a stool; also called accidental bowel leakage.
• Fistula: An abnormal connection between body parts, commonly developing between different organs, such as the bowel and vagina; can be caused by injuries, infections, complications from surgery, and diseases, such as Crohn disease and ulcerative colitis.
• Gastroenteritis: Inflammation of the intestinal lining; caused by a virus, bacteria, or parasites. Viral gastroenteritis is a very common illness.
• Hirschsprung disease: Congenital disorder caused by malformed intestinal nerves; also called congenital megacolon. Leads to severe constipation and intestinal obstructions.
• Intestinal ischemia and infarction: Occur when there is a partial or complete blockage in the arteries supplying the intestines. Can cause damage or death to the intestinal tissues.
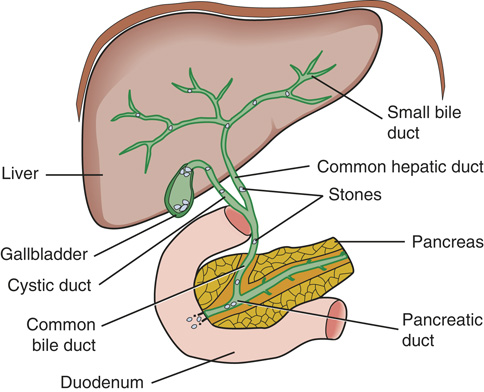
FIGURE 19.12 Gallstones.
• Intestinal volvulus: Occurs when the intestine twists around itself and the supporting mesentery, leading to an obstruction.
• Intussusception: Occurs when part of the intestine slides onto another portion of the intestine. It can cause an intestinal blockage. The blood supply may be constricted, leading to intestinal tissue death.
• Small intestinal bacterial overgrowth (SIBO): Caused when a large number of bacteria grow in the small intestine, which may use up important nutrients needed by the body, leading to malnourishment.
