Nutritional and Metabolic Health Pattern
June 23, 2023
Pica
Pica refers to craving and eating substances that are not normally considered edible. Although there are theories for this condition, none are proven. It is seen more in lower socioeconomic groups and linked to certain cultural groups. Incidence rates do spike with pregnancy as 20% of pica cases involve pregnant women (Kahn, 2010). Substances ingested may include clay, laundry starch, dirt, and chalk. Although the substances are not considered toxic, complications are associated with pica (Rose, 2000). Problems that may occur as a result of pica include interference with iron absorption, constipation, and loss of important nutrients when normal caloric intake is replaced with the pica-related substances.
Common Discomforts
Many pregnant women experience some discomforts of the gastrointestinal tract during pregnancy. Some women have excessive salivation (ptyalism), presumably in response to the high levels of estrogen during pregnancy. Although it may be uncomfortable and awkward at times, ptyalism causes no serious problems and disappears late in pregnancy or after delivery. Teach the patient to try using astringent mouthwash, chewing gum, or sucking on hard candy to provide relief.
Nausea is common in the early stages of pregnancy. It typically occurs when the woman awakens in the morning, hence, the name “morning sickness.” It can, however, occur at any time of the day. Nausea is thought to be caused by increased HCG levels and changes in carbohydrate metabolism. Mild nausea can usually be controlled by slowly eating a few soda crackers or dry toast before rising from bed. Other suggestions are eating smaller, more frequent meals and avoiding spicy or greasy food. Morning sickness rarely lasts beyond the 4th month. If it lasts longer, if it is more severe, and particularly if it involves vomiting, the health care provider should be contacted. The most severe form is called hyperemesis gravidarum. Its cause is not clear, but if left untreated, it can lead to dehydration, fluid and electrolyte imbalance, acid-base imbalance, altered kidney and cardiac function, and even fetal death. Hospitalization with close medical supervision, including intravenous therapy, may be necessary (see Chapter 28).
Pyrosis (heartburn) from gastric reflux into the esophagus can be caused by the increasing size of the fetus in the abdominal cavity, which displaces the stomach. Increased progesterone levels cause relaxation of the cardiac sphincter; decreased gastric mobility, which results in delayed stomach emptying time, can also contribute to the problem. Smaller, more frequent meals; decreased fat intake; low-sodium antacids; and avoidance of lying down after meals often give relief.
Skin Changes
Changes in pigmentation often occur during pregnancy as a result of increased amounts of melanocyte-stimulating
hormone. The changes occur primarily in areas that already have greater pigmentation, such as the areolae, nipples, vulva, and perineal area. A darkening of a line from the midline of the abdomen from the pubis to the umbilicus may result and is called the linea nigra.
Chloasma, the mask of pregnancy, is an irregular darkening of the cheeks, forehead, and nose. These changes are often more obvious in women with darker hair and skin and may be worsened with sun exposure. This generally disappears or fades significantly soon after delivery.
Striae gravidarum, or stretch marks, are reddish, wavy streaks that can appear on the thighs, the abdomen, and the breasts. They are more common with distention but may occur even in relatively thin women. They usually fade after delivery. Because integumentary system changes vary greatly among women of different racial backgrounds, the color of a woman’s skin along with any changes that may be attributed to pregnancy should be noted in the physical assessment.
Spider nevi (a branched growth of dilated capillaries on the skin) and palmar erythema (reddened palms) are sometimes seen. These conditions are caused by increased blood flow that results from high estrogen levels. Both usually disappear when the pregnancy ends.
Hair and nail growth are frequently accelerated during pregnancy, with hirsutism (excessive body hair in a masculine distribution pattern as a result of heredity, hormonal dysfunction, or medication) commonly reported. Oily skin and acne may occur in some women, whereas others report a clearing of their skin. This is usually temporary unless other physiologic problems are active.
Occasionally, decreased emptying of the gallbladder may result in subclinical jaundice, which causes generalized pruritus (itching). This and other concerns are noted in Table 25-4.
Changes in the Cardiovascular System
Maternal adjustments to pregnancy involve extensive changes in the cardiovascular system, both anatomic and physiologic. Changes can result in episodes of orthostatic hypotension. An increase of platelets and fibrinogen increases the woman’s risk for blood clots. Cardiovascular adaptations protect the woman’s normal physiologic functioning, meet the metabolic demands of pregnancy, and provide for fetal development and growth (Table 25-5).
Changes in the Respiratory System
Structural and ventilatory adaptations during pregnancy provide for maternal and fetal needs. Maternal oxygen requirements increase in response to the accelerated metabolic rate and the need to add to the tissue mass in the uterus and breasts. In addition, the fetus needs oxygen and a way to eliminate carbon dioxide. Elevation of estrogen causes the ligaments of the rib cage to relax, permitting increased chest expansion (Table 25-6).
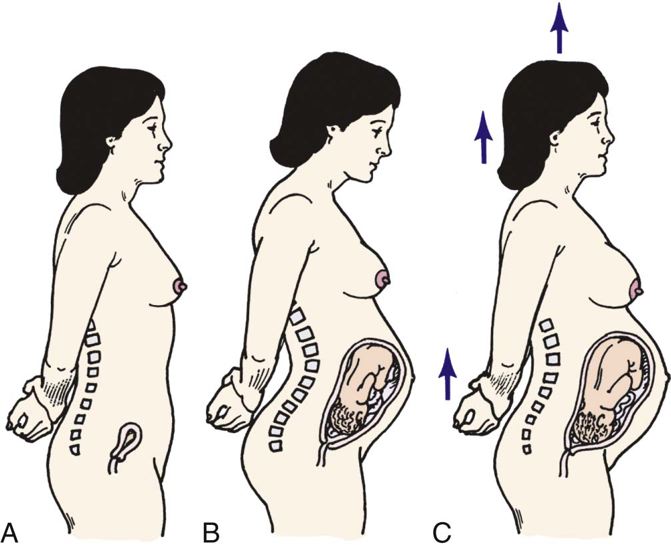
Changes in the Musculoskeletal System
The gradually changing body and increasing weight of the pregnant woman cause noticeable alterations in her posture (Figure 25-6) and the way she walks late in pregnancy. The great abdominal distention that gives the pelvis a forward tilt, decreased abdominal muscle tone, and increased weight bearing create a realignment of the spinal curvature. The woman’s center of gravity shifts forward. Lordosis (an increase in the normal lumbosacral curve) develops. An increased curvature in the cervicodorsal region is also seen. The expectant mother may also be noted with an exaggerated anterior flexion of the head. This is done to promote balance. As the pregnancy advances, common symptoms include muscle aches and numbness. Enlarging breasts and a stoop-shouldered stance further accentuate the lumbar and dorsal curves. Walking is more difficult, and the pregnant woman’s waddling gait is well known. The ligamentous and muscular structures of the middle and lower spine may be severely stressed. Pregnant women who gain excessive weight or who carry more than one fetus may experience overdistention. This excessive stress on the abdominal wall muscles may cause a separation (diastasis recti abdominis). Management of this condition is typically conservative, but severe cases may necessitate surgical repair.
Table 25-4 Discomforts and Concerns Related to Maternal Adaptations During the Third Trimester
DISCOMFORT | PHYSIOLOGY | TEACHING FOR SELF-CARE |
Shortness of breath and dyspnea in 60% of pregnant women | Expansion of diaphragm limited by enlarging uterus; diaphragm elevated approximately 1.5 inches (4 cm); some relief after lightening (when the fetus settles lower in the true pelvis, leaving more space in the upper abdomen) | Good posture; sleep with extra pillow; avoid overloading stomach; stop smoking; refer to physician if symptoms worsen to rule out anemia, emphysema, and asthma |
Insomnia (later weeks of pregnancy) | Fetal movements, muscular cramping, urinary frequency, shortness of breath, or other discomforts | Reassurance; conscious relaxation; back massage or effleurage (deep or gentle stroking); support of body parts with pillows; warm milk or shower before retiring |
Psychosocial responses: mood swings, mixed feelings, increased anxiety | Hormonal and metabolic adaptations; feelings about impending labor, delivery, and parenthood | Reassurance and support from significant other and nurse; improved communication with partner, family, and others |
Return of urinary frequency and urgency | Vascular engorgement and altered bladder function caused by hormones; bladder capacity reduced by enlarging uterus and fetal presenting part; lightening | Kegel exercises (see Patient Teaching box on Kegel exercises); limit fluid intake before bedtime; reassurance; wear perineal pad; refer to health care provider for pain or burning sensation |
Perineal discomfort and pressure | Pressure from enlarging uterus, especially when standing or walking; multifetal gestation | Rest, conscious relaxation, and good posture; maternity girdle; refer to physician for assessment and treatment if pain is present; rule out labor |
Braxton Hicks contractions | Intensification of uterine contractions in preparation for work of labor | Reassurance; rest; change of position; practice breathing techniques when contractions are bothersome; effleurage; rule out labor |
Leg cramps (gastrocnemius spasm), especially when reclining | Compression of nerves supplying lower extremities because of enlarging uterus; reduced level of diffusible serum calcium or elevation of serum phosphorus; aggravating factors: fatigue, poor peripheral circulation, pointing toes when stretching legs or when walking, drinking >1 quart (1 L) of milk per day; cause unclear | Assess lower extremities for redness, warmth, tenderness, or swelling; some facilities may use the Homan’s sign; this assessment is presently under review by many medical professionals as it is not considered completely reliable and concerns exist about the safety of the practice Heat may be used over affected muscle; stretch affected muscle until spasm relaxes |
Ankle edema (nonpitting) to lower extremities | Edema aggravated by prolonged standing, sitting, poor posture, lack of exercise, constrictive clothing (e.g., garters), or hot weather | Ample fluid intake for “natural” diuretic effect; put on support stockings before rising; rest periodically with legs and hips elevated; exercise moderately; refer to physician if generalized edema develops (diuretics are contraindicated) |
Slight relaxation and increased mobility of the pelvic joints are normal during pregnancy. They are a result of the exaggerated elasticity and softening of the connective tissue caused by increased circulating steroid sex hormones, especially estrogen. Relaxin, an ovarian hormone, assists in the relaxation and softening. These adaptations permit enlargement of pelvic dimensions to facilitate labor and birth. The degree of relaxation varies, but considerable separation of the symphysis pubis and the instability of the sacroiliac joints may cause pain and difficulty in walking. Obesity and multifetal pregnancy tend to increase the pelvic instability.
