Pancreatic Diseases and Disorders
April 11, 2024
Learning Objective: Examine pancreatic diseases and disorders, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Diabetes mellitus (DM) is the most common pancreatic disease. The following sections discuss type 1, type 2, and gestational diabetes.
Diabetes Mellitus
Learning Objective: Describe diabetes mellitus, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
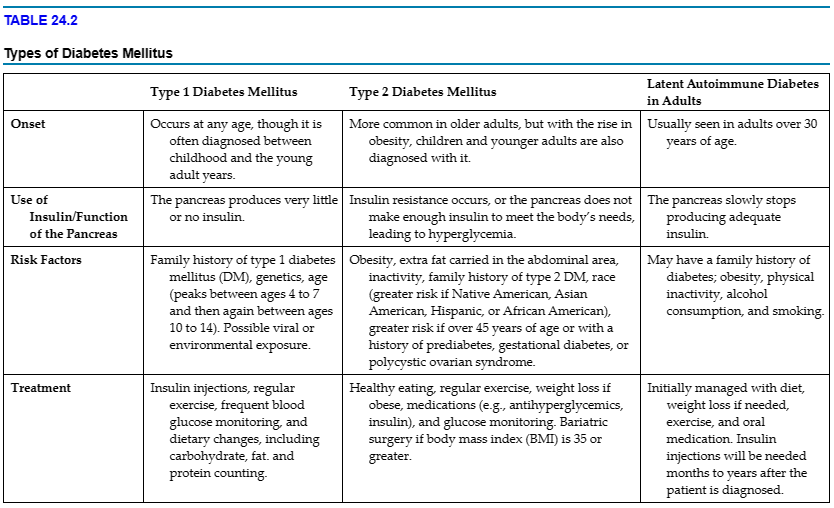
DM is a group of metabolic disorders characterized by an inadequate production of insulin, a resistance to insulin, or a combination of both. TABLE 24.2 describes type 1 DM, type 2 DM, and latent autoimmune diabetes in adults (LADA, sometimes called type 1.5 DM). (Gestational diabetes will be discussed in a separate section.)
The exact cause of DM is unknown. Type 1 DM and LADA are autoimmune conditions. The immune system destroys the beta islet cells of the pancreas. See TABLE 24.2 for risk factors for the different types of diabetes.
Signs and symptoms relate to hyperglycemia. With type 1 DM, the hyperglycemia can occur suddenly, whereas with type 2 DM and LADA it can be gradual. Hyperglycemia signs and symptoms include polydipsia, polyuria, polyphagia, weight loss, fatigue, blurred vision, frequent infections, and slow-healing wounds.
After a medical history and physical exam, the provider will order laboratory tests. The following diagnostic results suggest diabetes:
• Glycated hemoglobin (A1C) test, 6.5% or greater on two separate samples
• Fasting blood glucose test, 126 mg/dL or greater on two separate samples
• Oral glucose tolerance test, greater than 200 mg/dL for the 2-hour level
• Random blood glucose test, no matter when the person ate last, 200 mg/dL or greater and diabetes symptoms
See TABLE 24.2 for the treatments for each type of DM.
Hyperglycemia
With a fasting blood glucose test, the normal level is 70 to 99 mg/dL. Hyperglycemia occurs when the blood glucose level is elevated or above the normal limit. Blood glucose levels increase due to the following:
• Eating too many carbohydrates without enough insulin
• An infection, injury, or surgery, regardless of the amount of carbohydrates eaten
• Missing an insulin injection
Usually during an illness, people with type 1 diabetes mellitus have a special diabetic management plan to follow, which may include extra insulin and increased blood glucose monitoring.
24.7 Critical Thinking Application
Summarize the difference between type 1 and type 2 diabetes mellitus.
Complications of Diabetes Mellitus
According to the Centers for Disease Control and Prevention (CDC; www.cdc.gov), since the early 2000s, the number of people with DM has tripled. During that same time span, the top complications of DM—heart attack and stroke-have decreased because of the advances in DM education and care. The complications of diabetes mellitus develop over time. Two factors increase the risk of complications: the longer a person has DM the more uncontrolled the blood glucose is.
Diabetes affects the entire body. The following list provides a snapshot of possible complications of diabetes mellitus:
• Cardiovascular disease: People with DM have twice the risk of having a heart attack and stroke compared to people without diabetes mellitus. Diabetes increases the risk for coronary artery disease with angina (chest pain) and atherosclerosis (narrowing of the arteries).
• Blindness and eye conditions: Diabetic retinopathy, glaucoma, and cataracts can lead to vision loss. Early prevention and screening can prevent blindness with diabetic retinopathy. It is recommended that people with diabetes have their eyes checked every 4 to 6 months.
• Neuropathy: One of the most common complications of DM is nerve damage affecting the digestive system, reproductive system, cardiovascular system, and the extremities. Capillaries help nourish the nerves in the body, but hyperglycemia can damage the capillary walls, thus also causing nerve damage. Damage to the nerves in the gastrointestinal (GI) system can cause nausea, vomiting, constipation, or diarrhea. Men can have erectile dysfunction. A person with neuropathy can experience burning, tingling, pain, and numbness in the fingers and toes, which gradually move up the extremities. If left untreated, a loss of feeling in the extremities may occur, which can affect functioning.
• Poor healing of wounds: Diabetes also makes a person more susceptible to bacterial and fungal skin infections. With the lack of feeling in the extremities, the person is more at risk for foot sores, blisters, and cuts. Left untreated, they can become infected, which increases the blood glucose levels. This affects the healing process, which may lead to amputations to stop the spread of infection.
• Kidney disease: Hyperglycemia also damages the tiny blood vessels (glomeruli) in the kidney, leading to chronic kidney disease (CKD). Untreated CKD leads to kidney failure, which requires dialysis or a kidney transplantation.
• Dementia: Type 2 diabetes increases a person’s risk of dementia-related disorders (e.g., Alzheimer disease).
• Depression: This is common in patients with type 1 and type 2 DM.
• Periodontal disease: Gum infections and tooth loss can occur, which also increases hyperglycemia. It is recommended that patients with diabetes have dental cleanings and exams twice a year.
24.8 Critical Thinking Application
Cecilia is rooming Susie Westwood, who has had type 2 DM for 4 years. Cecilia asks Susie when she last had her eyes checked and had a dental exam. Susie could not remember and asked Cecilia why that was important. How would you answer Susie?
Gestational Diabetes
Learning Objective: Describe gestational diabetes, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Gestational diabetes develops during pregnancy. Hyperglycemia can affect the health of the pregnancy and the baby. Usually, after the pregnancy, gestational diabetes resolves, though there is a greater risk for type 2 DM.
The exact cause is unknown, though hormones produced by the placenta impair the action of insulin, leading to hyperglycemia. Risk factors include being older than age 25, having a family history of type 2 DM, having a personal history of prediabetes, being overweight, and race (risk is greater if one is Native American, Asian, Hispanic, or African American). There are no signs or symptoms of gestational diabetes.
A routine oral glucose tolerance test is usually done during weeks 24 to 28 of pregnancy. Treatment for gestational diabetes includes eating a healthy diet, monitoring blood glucose levels, regular exercise, insulin injections, and closer follow-up for both the patient and the baby.
Complications of Gestational Diabetes
Complications of gestational diabetes can include issues with the baby and the mother. The following complications can affect the baby:
• Excessive growth in utero: The extra glucose in the mother’s blood passes into the baby’s bloodstream, causing the baby’s pancreas to make extra insulin. This causes extra weight to be added to the baby, thus increasing the likelihood the child may need to be delivered by a C-section.
• Death: If the mother does not get treated for gestational diabetes, the risk of death for the baby during pregnancy or after birth increases.
• Hypoglycemia shortly after birth: With the extra insulin production in utero, the baby may be at risk for hypoglycemia shortly after birth.
• Risk of developing obesity and type 2 DM later in life.
For the mother, complications include preeclampsia and C-section delivery. She is at a greater risk for gestational diabetes with future pregnancies and having type 2 DM later in life.
Diabetic Ketoacidosis
Learning Objective: Discuss diabetic ketoacidosis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Diabetic ketoacidosis (DKA) is a life-threatening hyperglycemic condition more commonly seen in people with type 1 DM and LADA.
DKA occurs when there is not enough insulin in the body, which helps the blood glucose move to the cells. Because the cells need energy, the body starts rapidly breaking down fats, which leads to a buildup of ketones in the blood and urine, causing ketoacidosis. DKA can cause the following:
• Decreased alertness and headache
• Nausea, vomiting, abdominal pain, and dry mouth
• Muscle aches or stiffness, dry skin, and flushed face
• Frequent urination or thirst lasting for 1 or more days
• Fruity-smelling breath
Laboratory tests include blood glucose, urine, and blood ketones. A basic metabolic panel (which includes electrolytes [e.g., sodium and potassium] levels) may also be done. The goals of treatment are to correct the hyperglycemic level, replace lost fluids, and correct any electrolyte imbalances. Treatment usually consists of insulin, intravenous (IV) fluids, and frequent glucose and electrolyte monitoring. Sometimes, DKA treatment can be done in an ambulatory care facility; other times patients will be transported to the local emergency department for care.
Hypoglycemia
Learning Objective: Discuss hypoglycemia, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Hypoglycemia means low blood glucose (below 70 mg/dL). Hypoglycemia is commonly seen with DM but also can be seen with other conditions.
Hypoglycemia in DM usually occurs due to a medication side effect. A person takes too much insulin or oral medication for the amount of carbohydrates consumed, thus dropping the blood glucose level. Early hypoglycemia can cause irregular heart rhythm, pale skin, sweating, shakiness, and fatigue. The person may experience irritability, hunger, a tingling sensation around the mouth, and crying out while sleeping. As hypoglycemia worsens (the blood glucose level drops more), a person may experience behaviors that may be similar to being intoxicated:
• Visual disturbances and blurred vision
• Clumsy movements and seizures
• Confusion, abnormal behavior (e.g., incoherent speech, slurring words, inability to complete routine tasks), and loss of consciousness
Immediate treatment is required and involves increasing the blood glucose level. If people are alert and can swallow, they should follow the 15/15 rule. For an unconscious adult patient or child over age 6, glucagon 1 mL should be given subcutaneously or intramuscularly (IM) to treat hypoglycemia. This dose should be repeated in 15 minutes if the patient is still unconscious. Children younger than 6 years of age should receive glucagon 0.5 mL. The blood glucose should be monitored, and once the person is alert and able to swallow, additional food should be given.
15/15 Rule
People should eat 15 grams of fast-acting carbohydrates, and then wait 15 minutes before retesting their blood glucose level. This cycle should be followed until the blood glucose level returns to normal. At that time, the person should eat a small, balanced snack that contains both a protein and a carbohydrate if the next meal is more than 2 hours away. Examples of 15 grams of fast-acting carbohydrate include the following:
• 3 glucose tablets
• 4 ounces or ½ cup of fruit juice or regular soda (not diet soda)
• 6 to 7 hard candies
• 1 tablespoon of sugar
Additional Pancreatic Diseases and Disorders
Learning Objective: Describe additional pancreatic diseases and disorders.
Additional pancreatic diseases and disorders include the following:
• Hyperinsulinism: Hypersecretion of insulin; seen in some newborns of diabetic mothers. Causes severe hypoglycemia.
• Islet cell carcinoma: Also called pancreatic cancer; the fourth leading cause of cancer death in the United States. Treated with a Whipple procedure (pancreatoduodenectomy).
• Prediabetes: Condition in which the blood glucose level is higher than normal but not high enough for a diagnosis of type 2 diabetes.
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
