Patient Teaching: Preparing for Ultrasound Scan Examination
June 23, 2023
Inform the woman that she needs to have a full bladder for an abdominal ultrasound scan to allow better imaging of the fetus. Position her comfortably, with pillows under her head and knees, while the test is conducted. Apply ultrasonic gel to the abdomen and pass the scanner over it while images are reproduced. The woman and her partner can watch if they wish. The woman should not feel any discomfort.
For a transvaginal ultrasound scan, tell the woman that she may either be in a lithotomy position or have her pelvis elevated. These positions are optimal for imaging the pelvic structures. Introduce a transducer with a protective sheath covering into the vagina. If the woman wants to insert it herself, allow her to do so. The angle of the probe or the tilt of the table may be altered during the examination, but the procedure should not be painful.
structures. With the ultrasound scan, no definitive means exists to rule out the presence of chromosomal defects, which makes an amniocentesis an option for consideration by the mother and her healthcare provider.
Nuchal Translucency Testing
Nuchal translucency screening is a test that has grown in popularity since the late 1990s. It is a diagnostic procedure used to assess for potential Down syndrome. Fetuses with larger nuchal folds (thickness at the back of the neck) have a greater incidence of Down syndrome. The examination uses an ultrasound scan to measure the nuchal folds. The test is typically performed between 11 and 12 weeks gestation. A finding of excessive nuchal folds is not a definitive diagnosis for Down syndrome but indicates the need for additional testing such as an amniocentesis (U.S. National Library of Medicine, 2012).
Chorionic Villus Sampling
Chorionic villus sampling (CVS) is a test to detect genetic disorders of the fetus. It is usually performed at 8 to 12 weeks of gestation and requires aspiration of a small amount of tissue from the chorion of the placenta. A primary advantage of the test is the ability to perform it at an early point in the pregnancy, which allows for preparation of the mother in the event of fetal abnormalities. The test is associated with a slightly higher rate of pregnancy loss than the amniocentesis.
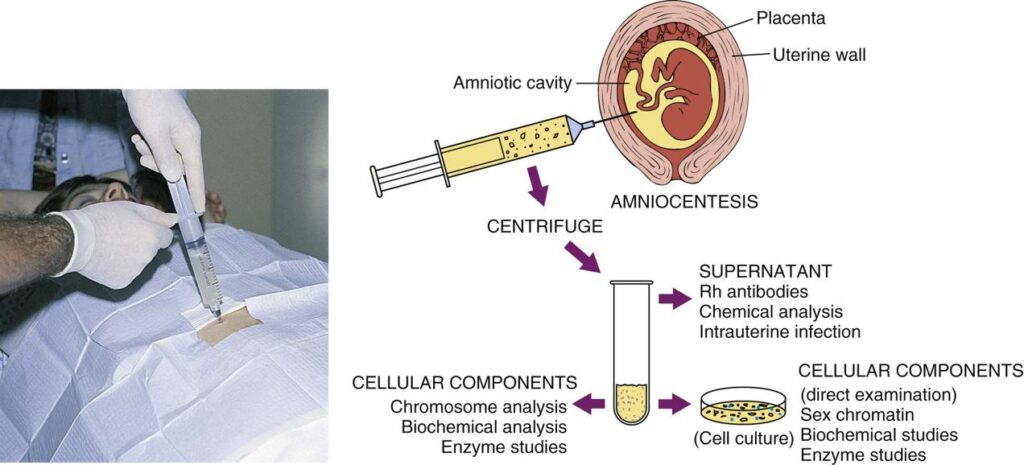
Amniocentesis
Amniocentesis involves removal of a small amount of amniotic fluid with a needle passed through the abdominal wall (Figure 25-3). This procedure is conducted in conjunction with abdominal ultrasound scan, which enables the physician to visualize the location of the fetus, the placenta, and a pocket of amniotic fluid. Laboratory examination of the amniotic fluid can reveal valuable information regarding genetic factors such as sex and chromosomal abnormalities, health status, and maturity of the fetus.
Early amniocentesis is performed at approximately the 16th week of pregnancy and is used to detect biochemical or chromosomal abnormalities. Testing at this time allows the mother to consider termination of the pregnancy before the legal point of viability is reached. The fetus’s ability to survive outside the uterus is known as viability. In the past several decades, the age of viability has decreased as a result of technological advances.
A fetus as young as 22 to 25 weeks gestation may survive outside of the mother’s womb. An important note is that babies born at this stage of the pregnancy face many physiologic challenges and potentially lifelong health deficits (MacDonald, 2002). Later in pregnancy, amniocentesis is primarily used to determine fetal lung maturity. It may also be performed to detect intrauterine infection and fetal distress and to assess fetal laboratory values.
Nonstress Test
The nonstress test (NST) is done to evaluate how the fetal heart rate responds to periods of fetal movement. It is indicated when a risk exists for placental insufficiency, such as pregnancy-induced hypertension, diabetes, postmaturity, maternal smoking, or inadequate maternal nutrition. It may also be done as a preventative screening tool for women who have had a past stillbirth. The test is often begun at 28 weeks gestation and beyond. It may be ordered as a single test or repeated weekly or biweekly, depending on the mother’s individual health history. With a baseline fetal heart rate of 120 to 160 bpm, the fetal heart rate normally accelerates at least 15 bpm for at least 15 seconds with fetal movement. Testing is done with external fetal monitors (see Chapter 26), with the tocotransducer recording fetal movement and the ultrasound transducer recording the fetal heart rate. A reactive result indicates a healthy fetus with findings of at least two fetal movements accompanied by two increases of 15 bpm in a 20-minute period. A nonreactive NST results when there is the absence of fetal heart increases with fetal movement. This may indicate a compromised fetus and requires further evaluation with another NST, a BPP, or a contraction stress test.
Nursing responsibilities include explaining the procedure to the patient, assuring the patient that no discomfort is associated with the NST, encouraging the patient to verbalize her fears, having the patient eat before the test to elevate serum glucose levels, having the patient empty her bladder and then assume a Sims position, applying the external fetal monitors to the patient’s abdomen, observing for an increase in fetal heart rate with fetal movement, and stimulating fetal activity with external methods if the fetus remains quiet for more than 20 minutes.
Contraction Stress Test
The contraction stress test (CST) or oxytocin stress test uses external fetal monitoring and stimulation of contractions to evaluate how the fetal heart rate responds to the decreased oxygen supply during uterine contractions. Contractions are elicited with the administration of oxytocin or nipple stimulation. The desired response is termed negative, which means that no change in fetal heart rate occurs with the contractions. A positive test is noted when the fetal heart rate declines with the contractions. A drop in fetal heart rate indicates placental insufficiency and fetal hypoxia. Declines in fetal heart rates are identified by where in the cycle of the contraction they occur. Declines in the heart rate at or after the midpoint of the contraction are referred to as late decelerations. Late decelerations are considered an ominous sign. The fetus may be at risk during labor and need delivery via cesarean section.
Magnetic Resonance Imaging
Magnetic resonance imaging (MRI) is a noninvasive tool that can be used for obstetric and gynecologic diagnosis. As with computed tomographic (CT) scan, MRI provides excellent pictures of soft tissue. Unlike CT scan, ionizing radiation is not used; thus, vascular structures within the body can be evaluated without injection of an iodinated contrast medium, thereby eliminating any known biologic risk. As with sonography, MRI is noninvasive and can provide images in multiple planes, but interference from skeletal, fatty, or gas-filled structures is not a problem. Also, imaging of deep pelvic structures does not depend on a full bladder. Although this procedure has many advantages, its total safety has not been accurately determined.
Biophysical Profile
The BPP assesses fetal status with evaluation of several factors (Table 25-3). These include the NST, fetal breathing movements, fetal muscle tone, fetal movements, and amniotic fluid volume. Each category is given a score of 0 or 2. A total score of 8 or more is reassuring; lower scores may warrant interruption of the pregnancy.
