Skeletal System Diseases and Disorders
April 11, 2024
Skeletal System Diseases and Disorders
Learning Objective: Examine skeletal diseases and disorders, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
The skeleton, muscles, and joints together work as a unit to move the body. Diseases and disorders of the musculoskeletal system often affect the ability to move with ease. Here are some common signs and symptoms of musculoskeletal disorders:
• Inflammation
• Pain or swelling in the joints or bones
• Temporary loss of function or loss of normal mobility
The following sections describe in detail some of the more common diseases seen in the ambulatory care setting. Conditions affecting the skeletal system, joints, and muscular system will be described.
Fractures
Learning Objective: Discuss fractures, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
A fracture is a broken bone. With an open (or compound) fracture, the skin is broken above the fracture (FIGURE 20.9A). With a closed (or simple) fracture, the skin is not broken, and no wound is visible (FIGURE 20.9B). Fractures can also be classified by the type of damage to the bone:
• Incomplete: The fracture line does not go across the entire cross section of the bone.
• Complete: The fracture line goes across the entire cross section of the bone (FIGURE 20.9C).
• Displaced: The bone fragments are not in alignment.
• Nondisplaced: The bone fragments remain in alignment.
• Comminuted: The bone breaks into three or more fragments.
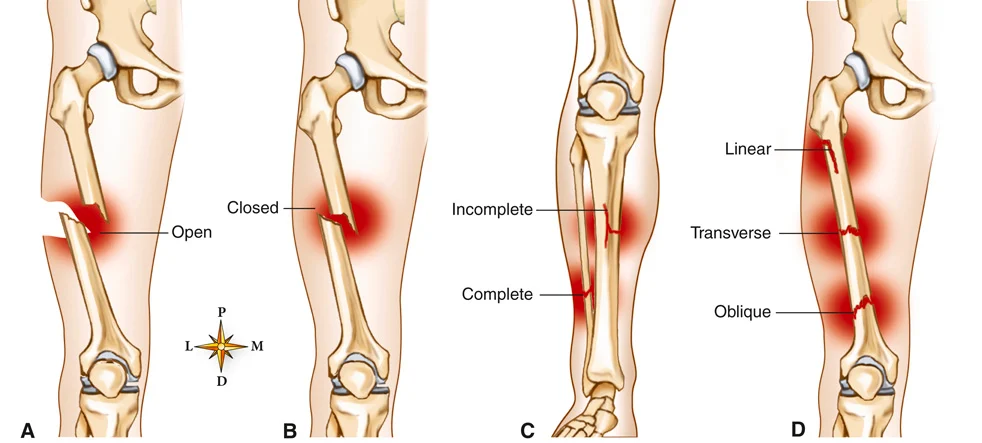
FIGURE 20.9 Bone fractures. (A) Open. (B) Closed. (C) Incomplete and complete. (D) Linear, transverse, and oblique. From Patton KT, Thibodeau GA: The human body in health and disease, ed 7, St. Louis, 2018, Elsevier.
• Compression: The fracture results in the bone (e.g., vertebrae) collapsing.
• Greenstick: The bone breaks on one side and is bent but still intact on the other side; commonly seen in children.
• Impacted: The bone fragments are driven into each other.
• Linear or longitudinal: The fracture line runs along the length of the bone (FIGURE 20.9D).
• Oblique: The fracture runs at an oblique angle across the bone.
• Pathologic (or spontaneous): The fracture is due to weakening of the bone structure by a pathologic condition.
• Spiral: The fracture line resembles a spiral; caused by the bone being twisted.
• Transverse: The fracture runs perpendicular across the bone.
Fractures can occur from trauma, overuse, or diseases. A pathologic fracture results from an underlying disease, such as osteoporosis or cancer. Signs and symptoms of a fracture include pain, swelling, bruising, numbness or tingling, deformity, and difficulty using or inability to use the affected area. Bleeding at the site of the break will also occur with compound fractures.
Most commonly, the provider will order an x-ray, but a bone scan, computed tomography (CT) scan, or magnetic resonance imaging (MRI) may also be used as a diagnostic test for some types of fractures. Depending on the type of fracture, treatment may include a cast, splint, or brace to immobilize the area. Surgery will be done if the bones are not aligned. During an open reduction and internal fixation (ORIF) surgery, the surgeon reduces (repositions and aligns) the bones and uses internal fixators (special metal devices [rods, screws, plates]) to hold the bones in place during the healing process (FIGURE 20.10). Sometimes, external fixators and traction are used to hold the bones in place. Medications may also be prescribed depending on the severity of the fracture. The provider may order analgesics for the pain, anti-inflammatory drugs, and muscle relaxants. Fractures may take several weeks to months to heal. Crutches or other assistive devices may be used for lower extremity fractures. A sling is used for an upper extremity fracture. Physical therapy may be ordered once the fracture is healed to strengthen the extremity.
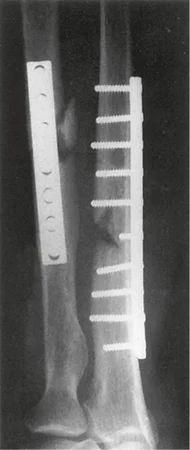
FIGURE 20.10 Orthopedic hardware from open reduction of fractures of the radius and ulna. From Mettler MA: Essentials of radiology, ed 3, Philadelphia, 2004, Saunders.
20.6
Critical Thinking Application
A patient comes into the clinic hopping on one foot and holding the other in the air. She thinks she broke her ankle when she stepped off the curb wrong and fell. What tests will Dr. Kahn most likely order? Why?
Herniated Disk
Learning Objective: Discuss a herniated disk, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
When one of the soft disks between the vertebrae has a crack, some of the jelly-like substance can leak out (FIGURE 20.11). This is called a ruptured, slipped, or herniated disk. The leaking jelly-like substance can lead to inflammation and compression of the local nerve.
The disks can degenerate with age. Middle-aged and older men are more at risk for a herniated disk. Typically, herniation occurs with strenuous activities, but it can also occur with lifting heavy objects, obesity, repetitive movements involving the lower back, long periods of sitting or standing, inactivity, and smoking. Signs and symptoms of a lower back herniated disk include sciatica (pain and numbness from the hip down to the foot), back pain, and weakness. The pain usually starts slowly and gets worse with standing or sitting. A herniated disk in the neck may cause pain and numbness from the shoulder down to the fingers.
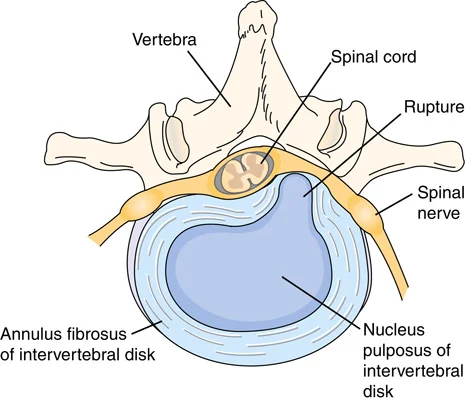
FIGURE 20.11 Herniation of a vertebral disk.
The provider will check the patient’s reflexes and muscle strength. The provider may order diagnostic tests (e.g., myelogram and electromyography [EMG]) and imaging procedures (e.g., spine MRI, spine CT, and spine x-ray). The following are common treatments:
• Medications (e.g., nonsteroidal anti-inflammatory drugs [NSAIDs], narcotics, and muscle relaxants) to help reduce the pain, inflammation, and muscle spasms
• Rest and physical therapy
• Surgery to remove the herniation if the symptoms remain unchanged
Usually, the condition improves in 4 to 6 weeks.
Lordosis, Kyphosis, and Scoliosis
Learning Objective: Discuss lordosis, kyphosis, and scoliosis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
The spine has normal curves (FIGURE 20.12). Abnormal curvatures of the spine deprive the body of important features related to spinal strength, balance, and posture. The three most common curvatures are as follows:
• Lordosis (swayback): An exaggerated forward curve in the lumbar region, which makes the buttock appear larger (FIGURE 20.13A)
• Kyphosis (hunchback): An exaggerated curve in the thoracic region (FIGURE 20.13B)
• Scoliosis: An abnormal side-to-side (S or C) curvature that could be in both the thoracic and lumbar regions of the back (FIGURE 20.13C)
Lordosis is caused by genetic and congenital conditions (e.g., muscular dystrophy, spondylolisthesis). Kyphosis can occur at any age, but it more commonly occurs in adults due to degenerative diseases of the spine, fractures, and injury. Kyphosis can also be caused by Paget disease, muscular dystrophy, scoliosis, and tumors. Many times, scoliosis occurs in children from age 10 to early teens, and the cause is unknown. Abnormalities in any of the spinal curves can cause pain and fatigue in the lower back and legs. Lordosis can also cause pain that may affect mobility. Mild kyphosis may cause few symptoms, but severe kyphosis can cause back pain, stiffness, and an abnormally curved spine. Scoliosis can cause uneven shoulders and waist. One shoulder blade may be more prominent, and one hip may be higher than the other.
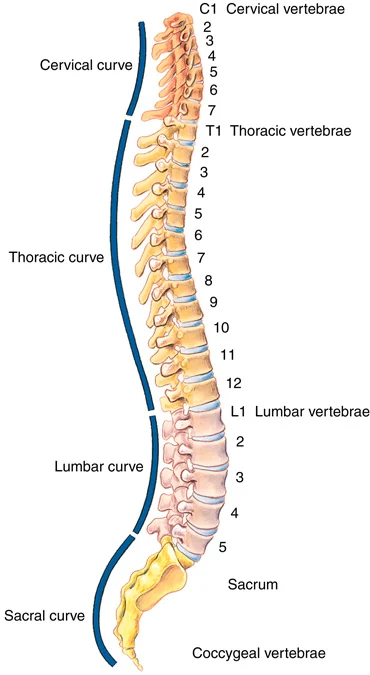
FIGURE 20.12 Normal curves of the spine. From Applegate E: The anatomy and physiology learning system, ed 4, St. Louis, 2011, Saunders.
The provider will perform a physical exam of the spine and a neurologic exam. A spinal x-ray, an MRI, and CT scan are also used as diagnostic tools. The treatment depends on the severity of the curve and the patient’s age and condition. Treatments include physical therapy, medications (analgesics, NSAIDs, steroids, and muscle relaxants), spinal fusion surgery, and a back brace; surgical placement of metal stabilizing rods may be needed for scoliosis. In most cases, with treatment, the prognosis is good.
Osteomalacia and Rickets
Learning Objective: Describe osteomalacia and rickets, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Osteomalacia is the softening of bones due to the lack of vitamin D. Vitamin D helps the body absorb calcium. Calcium is needed for strong bones. Osteomalacia occurs in adults and children; in children, this disease is called rickets.
Osteomalacia and rickets are caused by a lack of vitamin D, which can be related to an absorption issue (e.g., after gastric bypass surgery) or a lack of dietary intake. Osteomalacia can also be related to kidney failure, liver disease, and certain medications (e.g., anticonvulsants). Signs and symptoms include bone fractures without related injuries, muscle weakness, and widespread bone pain, usually in the hips.
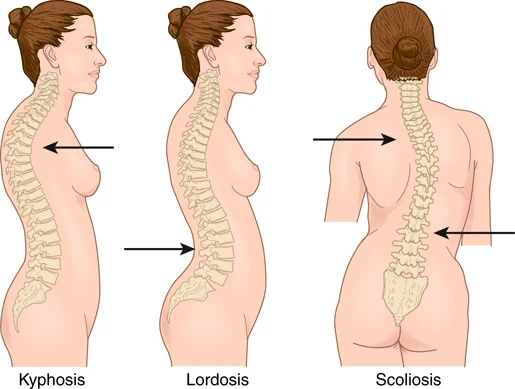
FIGURE 20.12 Normal curves of the spine. From Applegate E: The anatomy and physiology learning system, ed 4, St. Louis, 2011, Saunders.
The provider will order blood tests to check the vitamin D level, along with creatinine, electrolytes (e.g., calcium, phosphate), alkaline phosphatase, and parathyroid hormone levels. Bone x-rays, a bone density test, and a bone biopsy may be done. Treatment involves oral supplements of vitamin D, calcium, and phosphorus. Sunlight for vitamin D production is also recommended. With early treatment, the prognosis for rickets in children is excellent. The prognosis for osteomalacia is good if the vitamin D deficiency is addressed.
Osteoporosis
Learning Objective: Describe osteoporosis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Osteoporosis is a condition that causes bones to become brittle and weak. Healthy bone is constantly being broken down and remodeled. When a person has osteoporosis, bones are being broken down more quickly than new bone can be created. This leads to weak bones that are easily fractured, especially in the wrist, hip, and spine.
As people age, bone mass is lost faster than it can be produced, leading to osteoporosis. Increased risks for osteoporosis include menopause, family history, small body frame, white or Asian descent, hormonal imbalance, dietary deficiencies (low calcium intake), long-term corticosteroid use, celiac disease, kidney or liver disease, cancer, and some autoimmune conditions. A sedentary lifestyle, tobacco use, and excessive alcohol consumption are also risk factors for osteoporosis. Early osteoporosis is asymptomatic, but as the bones become weaker, back pain, height loss, stooped posture, and fractures can occur.
A bone density test is the only diagnostic tool for osteoporosis. This low-level x-ray determines the mineral content of the bone. The following treatments are used for osteoporosis:
• Weight-bearing exercises to maintain bone density
• Modifying risk factors to prevent falls
• Appropriate calcium and vitamin D intake from food or supplements
• Medications, such as bisphosphonates and hormone replacement therapy (estrogen)
Osteoporosis is a chronic condition that can be managed but does progress with age.
Healthy, Strong Bones
Peak bone mass is usually achieved around age 30. After that time, a little more bone is lost through remodeling than what is gained. This leads to a decrease in bone mass or density. For good bone health, it is important to do the following:
• Eat a diet rich in calcium. Good sources of calcium include dairy products, canned salmon with bones, soy products (e.g., tofu), broccoli and kale, and almonds.
• Take in adequate amounts of vitamin D. Vitamin D helps the body absorb dietary phosphorus and calcium. Good dietary sources of vitamin D include oily fish (e.g., trout, tuna, salmon), mushrooms, eggs, and fortified cereals and milk. Sunlight also helps in the body’s production of vitamin D.
• Limit tobacco and alcohol use. Tobacco use can lead to weak bones. Drinking more than one alcoholic drink per day for women and two for men can increase bone density loss.
• Do weight-bearing exercises. Weight-bearing exercises, such as jogging, climbing stairs, and walking, help build strong bones and slow bone loss.
20.7
Critical Thinking Application
Mrs. Viola Carson, a 78-year-old patient, is being seen in the office today for follow-up after hip replacement surgery. Mrs. Carson fractured her hip in a simple fall at the grocery store. Why would the physician suspect she has osteoporosis? What treatment might be recommended to prevent further fractures in this patient?
Spinal Stenosis
Learning Objective: Describe spinal stenosis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Spinal stenosis is the narrowing of the spine. The stenosis puts pressure on the nerves and spinal cord. Usually, spinal stenosis occurs in people over age 50, but it can affect younger people with spinal injuries. Cervical stenosis causes narrowing of the cervical spine in the neck. Lumbar stenosis causes narrowing of the lumbar spine in the lower back.
Causes of spinal stenosis include overgrowth of bone, herniated disks, tumors, spinal injury, and thickening of ligaments. Cervical spinal stenosis causes numbness, tingling, and weakness in the extremities. Neck pain, difficulty walking, and bowel and bladder incontinence can occur. With lumbar spinal stenosis, a person can experience weakness, tingling, numbness, cramping, and pain in the legs and feet. It can also cause back pain.
After an exam, the provider may order x-rays, an MRI, and a CT scan. Sometimes a CT myelogram is done. With a CT myelogram, a contrast dye is injected, which outlines the spinal cord and nerves, showing abnormalities. Spinal stenosis can be treated with surgery, analgesics, physical therapy, and steroid injections.
Paget Disease
Learning Objective: Discuss Paget disease, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
Paget disease is also called osteitis deformans. Paget disease causes abnormal bone destruction and regrowth. The new bone is larger but weaker, leading to deformities. Often the bones in the arms, legs, spine, skull, pelvis, and collarbones are involved.
The etiology is unknown. It may be related to genetic factors or a viral infection. Most patients experience no symptoms. If symptoms occur, the person may experience bone pain, joint stiffness and pain, and fractures. Deformities, such as an enlarged skull and bowing of the legs, can occur. A person can experience a reduction in height, kyphosis, and spinal stenosis. Hearing loss can also occur.
After an examination, the provider may order a bone scan and x-rays. Laboratory tests such as alkaline phosphatase (ALP), bone-specific isoenzyme, and serum calcium may be performed. Not all patients with Paget disease need to be treated. Patients with deformities and other symptoms may be treated with medications to reduce bone remodelings, such as bisphosphonates and calcitonin. For lumbar spinal stenosis due to a thickened ligament, percutaneous image-guided lumbar decompression (PILD) can be done. For this procedure, needle-like instruments are used to remove parts of the thickened ligament, thus widening the narrowed spinal canal.
Plantar Fasciitis
Learning Objective: Discuss plantar fasciitis, including the signs, symptoms, etiology, diagnostic procedures, and treatments.
The plantar fascia is a tough fibrous tissue that connects the toes to the heel on the bottom of the feet, creating the arch of the foot. Plantar fasciitis occurs when the plantar fascia becomes inflamed or swollen from being overstretched or overused. Plantar fasciitis is one of the most common foot issues.
People with flat feet or high arches are at risk for plantar fasciitis. Other risk factors include running long distances, obesity, wearing shoes with poor arch support, and having a tight Achilles tendon. Signs and symptoms include foot pain immediately in the morning, after standing, sitting, or intense exercise, and when climbing stairs. The pain can be on the bottom of the foot or along the sole of the foot. Mild foot swelling, redness, or stiffness can also be seen.
The provider will do an examination. A foot x-ray may be ordered to rule out other issues. Treatment involves over-the-counter analgesics, heel and foot stretches, and good arch supports in shoes. Severe cases may require immobilization, custom-made shoe inserts, steroid injections in the heel, and surgery. Plantar fasciitis usually resolves with treatment.
Additional Skeletal System Disorders
There are many skeletal disorders. The following are some examples:
• Amputation: The removal of a leg, foot, toes, fingers, or arm as a result of a trauma, accident, poor blood flow to the extremity, uncontrolled or worsening infection, tumor, or severe frostbite or burn. Risks of amputations include blood clots, bleeding, infection, poor surgical wound healing, and phantom sensations. After a limb is removed, a person may feel that the limb is still there. This can include experiencing numbness, hot or cold sensations, and pain (called phantom pain) in the limb that is no longer there. Depending on the type of amputation, many amputees use an artificial limb. Recovering from an amputation may require physical therapy, treatment with medicine, or counseling to help deal with sadness, anger, and frustration.
• Chondrosarcoma: A rare type of cancer that begins in bones or soft tissue near the bones.
• Ewing sarcoma: A rare type of cancer that starts in the bone or soft tissue near the bone. More common in children and teenagers.
• Fibrous dysplasia: Abnormal fibrous tissue replaces bone, leading to weak bones.
• Mastoiditis: Infection of the mastoid bone, commonly related to middle ear infections (acute otitis media).
• Osteogenesis imperfecta: Also called brittle bone disease; a genetic condition that causes bones to fracture easily.
• Osteomyelitis: A bacterial or fungal infection of the bone that comes from the bloodstream, surgery, or an injury. Signs and symptoms include chills and fever. The infected area can be painful, warm, red, and swollen. Antibiotics and surgery, if needed to remove dead bone tissue, can be done to treat the infection.
• Osteosarcoma: Most common bone cancer in children but can occur in adults; usually found in large bones, although it can occur in any bone.
• Polydactyly: Often a genetic condition in which a person has more than five toes per foot or five fingers per hand. The extra digit is often poorly formed and is usually surgically removed.
• Spina bifida occulta: Mildest form of spina bifida; no spinal nerves are involved, but one or more vertebrae are malformed; no signs or symptoms may be present. The only indication may be an abnormal cluster of hair, a small dimple, or a birthmark on the infant’s back.
• Spondylolisthesis: A forward displacement of a vertebra over the one below it; usually occurs in the lumbar or sacral area; can be related to a birth defect or acute trauma.
• Syndactyly: The digits (fingers and toes) are fused together or are webbed together. Most commonly seen with the second and third toes.
• Talipes (clubfoot): Most common congenital disorder of the legs; one foot or both feet are turned inward and downward; the calf and foot may be slightly smaller; treatment depends on the severity and can include stretching, casting, braces, and surgery.
