The Medical Assistant’s Role in Examinations, Diagnostic Procedures, and Treatments
April 11, 2024
Learning Objective: Examine the medical assistant’s role in examinations, diagnostic procedures, and treatments for endocrine diseases and disorders.
Endocrine diseases and disorders are common in primary care and endocrinology departments. Medical assistants help the provider with examinations, diagnostic procedures, and treatments.
Assisting with the Examination
Learning Objective: Describe the medical assistant’s role in examinations for endocrine diseases and disorders.
When the medical assistant is rooming a patient, it is important to accurately measure the vital signs and obtain the medical history. Encouraging the patient to voice any concerns or issues is vital. The medical assistant may be required to ask specific screening questions. Peripheral neuropathy screening questions for patients with DM may include the following:
• Do you have tingling, burning, numbness, cramps, or sharp pains in your hands and feet?
• Do you have a reduced ability to feel temperatures or pain in your hands and feet?
• Are your hands or feet more sensitive to touch?
• Do your hands or feet feel weaker?
• Do you have any problems with loss of balance or coordination?
• Do you have any sores, blisters, or any concerns with your feet?
When completing the medication section of the medical history, the medical assistant must verify the medication name, the dose amount, and the number of doses taken each day. Sometimes the information in the health record is different from what the patient is really doing. Having accurate information in the health record helps the provider evaluate the complete picture of the patient’s health.
During the physical exam, the provider often needs to examine the patient’s feet for any abnormalities. The medical assistant should assist the patient in removing shoes and socks as needed. For infection control purposes, the patient’s bare feet should never touch the floor. The medical assistant should place a piece of paper towel or some other barrier between the patient’s feet and the floor.
Peripheral Neuropathy Screening
Many providers have medical assistants perform peripheral neuropathy screening by doing the monofilament foot exam. This is commonly done for diabetic patients but needs to be done for any patient experiencing peripheral neuropathy symptoms. Procedure 24.1 describes the monofilament foot exam procedure.
Assisting with Diagnostic Procedures
Learning Objective: Describe the medical assistant’s role in diagnostic procedures for endocrine diseases and disorders.
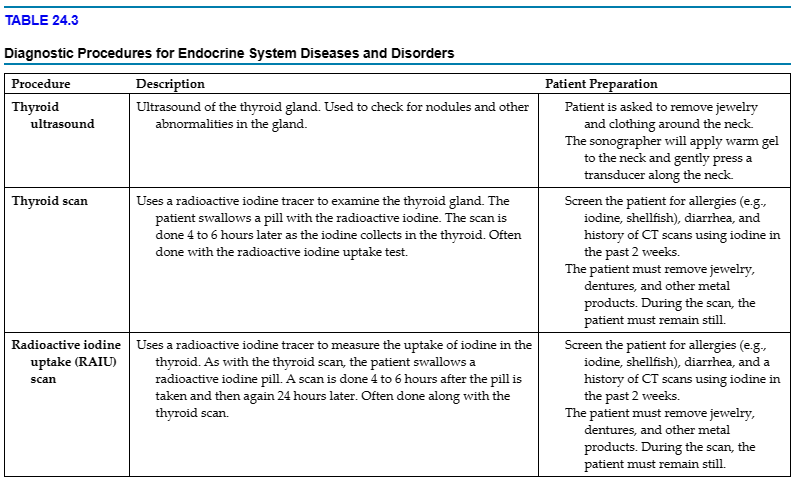
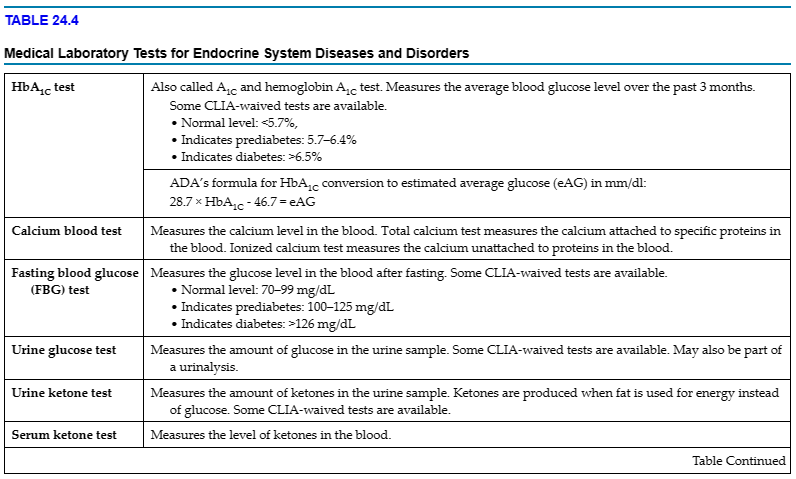
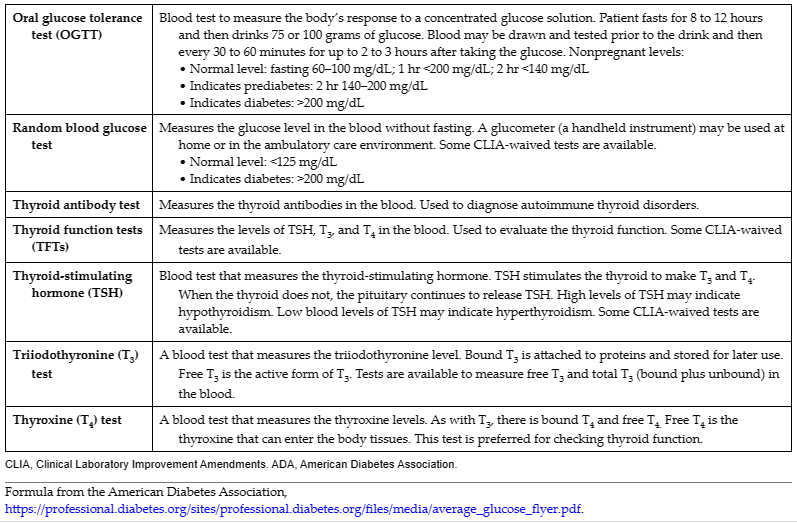
Tables 24.3 to 24.4 provide information about common diagnostic procedures and medical laboratory tests done for endocrine conditions. The medical assistant may be responsible for coaching patients on diagnostic procedures done in other departments. As with other diagnostic procedures, the medical assistant should coach the patient regarding the following:
• Patient preparation (e.g., dietary restrictions and medications to hold)
• Location and time of the test
• What to expect during the procedure
• Any follow-up required after the procedure
Assisting with Treatments
Learning Objective: Describe the medical assistant’s role in treatments for endocrine diseases and disorders.
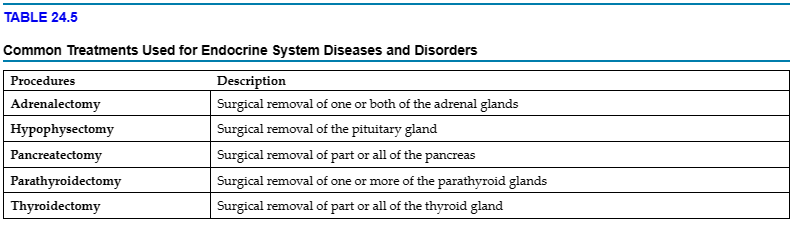
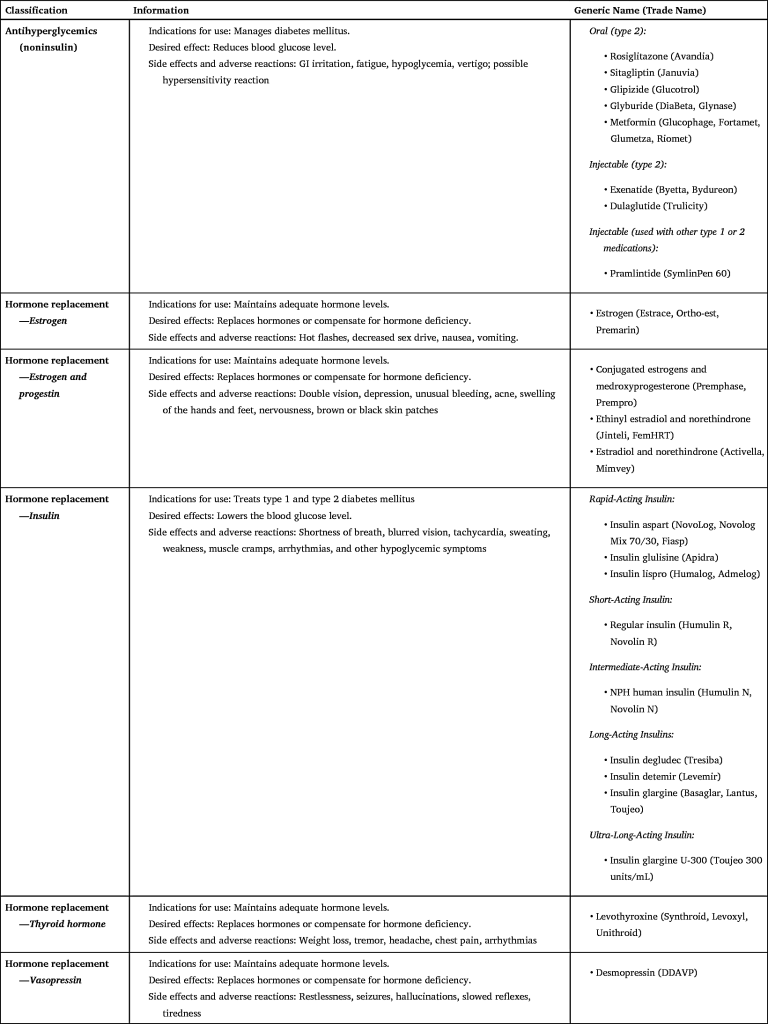
Some endocrine disorders are treated with surgery (TABLE 24.5). Many endocrine disorders are treated with medications. The following are some of the more common classifications of medications:
• Antihyperglycemic: Used to manage diabetes mellitus
• Hormone replacement: Used to maintain adequate hormone levels
• Estrogen: Used for menopause
• Estrogen and progestin: Used for menopause
• Insulin: Used to treat type 1 and type 2 diabetes mellitus
• Thyroid hormone: Used for hypothyroidism
• Vasopressin: Used for diabetes insipidus
Refer to TABLE 24.6, Medication Classifications, for information on drug classification, including indication for use, desired effect, side effects, adverse reactions, and generic and trade names. Medical assistants should be familiar with medications that are prescribed to patients.
In the ambulatory care facility, when a patient is prescribed insulin for the first time, the medical assistant may need to do some coaching if the patient is not seeing a diabetic educator immediately. If it is within the scope of practice for the medical assistant, the following topics should be addressed with the patient:
• How to draw up and give an insulin injection (discussed in Chapter 30)
• Signs and symptoms of hyperglycemia and hypoglycemia
• Immediate treatments for hyperglycemia and hypoglycemia
• How to use a glucometer to monitor blood glucose levels (discussed in Chapter 49)
• When to contact the provider or seek additional care
• Storage of supplies and how to discard used needles
Insulin
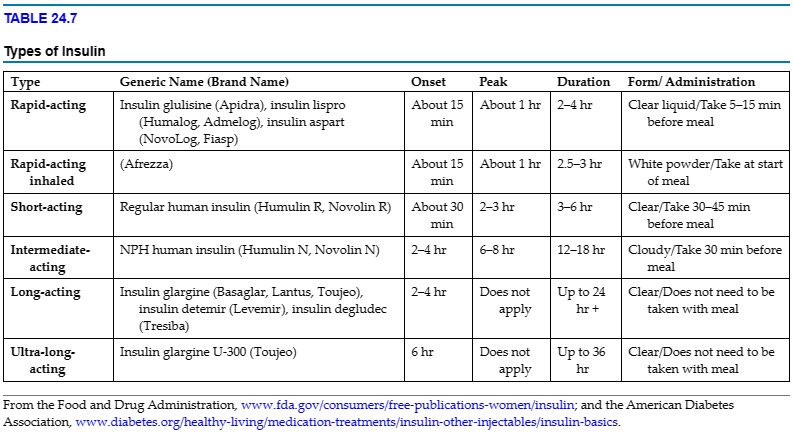
Insulin is used to treat type 1 and, in some cases, type 2 diabetes mellitus. Most commonly, insulin is injected subcutaneously several times a day. TABLE 24.7 describes the different types of insulins. The onset is the length of time before the insulin begins to work. The peak is the period when the insulin is most effective. The duration is the length of time the insulin exerts an effect on the body.
Many people take two types of insulin a day. Premixed insulins available in the United States include the following:
• Premixed—Intermediate- and rapid-acting: 75% insulin lispro protamine, 25% insulin lispro (Humalog Mix 75/25); 50% insulin lispro protamine, 50% insulin lispro (Humalog Mix 50/50); and 70% insulin aspart protamine, 30% insulin aspart (NovoLog Mix 70/30)
Medication Classifications
• Premixed—Intermediate- and short-acting: 70% NPH, 30% regular insulin (Novolin 70/30, Humulin 70/30)
• Premixed—Long- and rapid-acting: 70% insulin degludec, 30% insulin aspart (Ryzodeg 70/30)
Insulin can be given in the following ways:
• Syringe and vial: Insulin is drawn up in the syringe, and then the injection is given. Adaptive equipment is available to help patients see the calibration lines on the syringe.
• Insulin pump: This is a computerized device that administers insulin through a needle-tipped catheter attached to tubing and the medication container. The needle can be inserted in several locations, including the abdomen, outer thigh, back of the arm, hip, and buttock. The pump is programmed to deliver a basal rate, or the continuous infusion of a small dose of insulin over a 24-hour period. The person can also set the pump to deliver extra insulin to cover the carbohydrates being consumed. This method more closely resembles the body’s normal surge of insulin and is designed to maintain blood glucose levels consistently within normal limits.
• Injector pen: An injection device that is preloaded with insulin cartridges for easy use (FIGURE 24.13). Insulin pens are disposable or refillable and easily portable and therefore can be used by patients with diabetes when they are away from home.
• Inhaler: A cartridge containing the insulin is loaded into the inhaler. The person breathes in the insulin.
24.9 Critical Thinking Application
Explain why it is important for patients who take insulin to be aware of the onset, peak, and duration of the insulin.
Insulin Strengths
U-100 is the most common insulin strength in the United States. U-100 means that 100 units of insulin are dissolved or suspended in each milliliter (mL) of fluid. Additional insulin strengths are more concentrated.

FIGURE 24.13 NovoPen
• Humalog KwikPen contains 200 units of insulin per mL (U-200 insulin).
• Insulin glargine U-300 (Toujeo) contains 300 units of insulin in each mL of fluid or three times the amount of insulin compared to U-100 insulin.
• Humulin R U-500 contains 500 units of insulin in each mL of fluid or five times the amount of insulin compared to U-100 insulin.
More concentrated forms of insulin require additional patient education and special equipment (e.g., syringes or pens) to prevent insulin overdoses.
Storage of Insulin
Most insulin manufacturers recommend that insulin should be stored in the refrigerator. Because injecting cold insulin is uncomfortable, usually, the vial being used is stored at room temperature. An insulin vial stored at room temperature will last for about 1 month. It is important to keep insulin away from extreme heat or cold (e.g., freezer, direct sunlight, or in the glove compartment of a vehicle).
Afrezza, the inhaled insulin, should be stored in the refrigerator in the original closed container. Before using, the cartridge should warm at room temperature for 10 minutes. At room temperature, unopened medication packs are good for 10 days. Once the pack is opened, the cartridges are good for 3 days. The inhaler can be used for up to 15 days before it must be discarded.
