The Medical Assistant’s Role in Examinations, Diagnostic Procedures, and Treatments
April 11, 2024
The Medical Assistant’s Role in Examinations, Diagnostic Procedures, and Treatments
Learning Objective: Examine the medical assistant’s role in assisting with examinations, diagnostic procedures, and treatments for integumentary system conditions.
The integumentary system can reflect both internal and external reactions, disease processes. The skin holds information about the body’s circulation, nutritional status, and signs of systemic diseases. It also acts as a mirror, reflecting aging changes that occur in all organs of the body. For many people, self-esteem is linked to a youthful appearance, and dermatologic conditions may be very threatening to feelings of self-worth. As you prepare patients for a dermatologic examination, allow them to express their anxieties. The conditions that most frequently bring a patient to the dermatologist’s office are cosmetic disfigurements caused by a skin disease, pain and pruritus, and interference with sensations or movements.
Assisting with the Examination
Learning Objective: Describe the medical assistant’s role in assisting with examination for integumentary system conditions.
During a dermatologic examination, the provider inspects the entire body, beginning with the scalp and continuing to the soles, including the genital area. Inspection of the skin is followed by a detailed examination of suspicious areas through palpation, diascopy, and special tests. A diascope is a glass plate held firmly against the skin to permit observation of changes produced in underlying areas when pressure is applied. Inspection may include using a magnifying lens and a bright light to closely examine a suspicious lesion or growth. Dermatologists frequently ask medical assistants to take photographs of moles or to document specific measurements and locations of suspicious lesions. These are placed in the health record for comparison when the patient returns for follow-up visits.
In the physical examination, concerns about the integumentary system include abnormal colorings, such as cyanosis, pallor, vitiligo, erythema, leukoderma, or excessive brown patches. Jaundice may indicate an increase in the level of bilirubin in the blood. Lesions, ulcers, and bruises may be the result of pathologic conditions. Localized red or purple discoloration may be caused by vascular neoplasms, birthmarks, or subcutaneous hemorrhages (petechiae and ecchymosis). Palpation helps confirm the findings of the inspection. Therefore, inspection and palpation are interrelated in confirming the diagnosis of an integumentary system disorder. Palpated findings may include the skin’s texture or elasticity or the presence of edema or a neoplasm.
Gowning and draping a patient for a skin examination depends on the area to be examined. Remember to expose the area adequately but also to protect the patient’s privacy. Try to make the patient as comfortable as possible and offer support when it is needed.
Assisting with the Examination
Learning Objective: Describe the medical assistant’s role in assisting with diagnostic procedures for integumentary system conditions.
The medical assistant is often involved in assisting with diagnostic procedures of the integumentary system. It is important to remain professional during these interactions. The following sections describe the medical assistant’s role in helping with those diagnostic procedures.
Tissue Biopsy
Three methods are used to obtain a small piece of tissue for examination under a microscope. In an excision biopsy, such as the removal of a mole, the entire lesion may be removed for analysis. A punch biopsy involves the removal of a small section from a designated location in the lesion; the center usually is the optimum site. If the lesion is on the surface of the skin (e.g., a mole), this is done with a scalpel-like circular punch instrument (FIGURE 17.21); in other cases, a large-gauge needle and syringe unit are used to aspirate cells and fluid from a suspicious area (e.g., a breast biopsy). A shave biopsy is performed with a scalpel or razor by cutting or shaving off the growth or lesion for a thin specimen of the combined epidermis and upper dermis cells. This method is used to biopsy a possible squamous cell carcinoma lesion. The medical assistant may help the provider perform these biopsy procedures.
The medical assistant should follow these steps to assist with a tissue biopsy:
1. Assemble the necessary supplies for the procedure.
2. Prepare the patient with proper gowning, draping, and positioning, and make sure the patient understands the procedure.
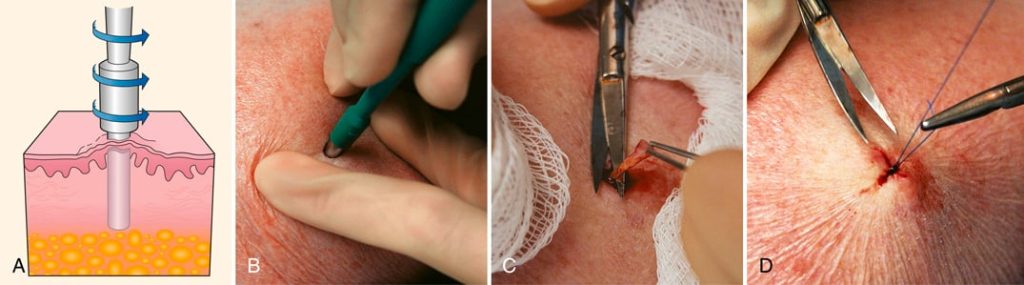
FIGURE 17.21 (A) Punch biopsy. (B) Punch biopsy instrument rotated into the skin. (C) Cutting the base of the specimen. (D) Closure of the biopsy wound with a simple epidermal stitch. Modified from Bolognia J: Dermatology, ed 2, Edinburgh, 2008, Mosby.
3. Confirm that the provider has obtained the patient’s informed consent.
4. Prepare the site of the biopsy according to office protocol.
5. Assist the provider as needed, using appropriate personal protective equipment according to Standard Precautions.
6. Label the sample container and prepare it for transport to the testing laboratory. Remember to include laboratory request forms.
7. Clean the procedure area, properly dispose of all waste materials, and disinfect and sterilize equipment used in the procedure.
8. Sanitize your hands and document the procedure, including the patient education provided on biopsy site care.
Assisting with Treatments
Learning Objective: Describe the medical assistant’s role in assisting with treatments for integumentary system conditions.
When working in dermatology, the medical assistant is often involved in assisting with the treatment of various integumentary conditions. The following sections discuss that role.
Burns
The treatment of burns will vary depending on the severity of the burn. Burns can be treated with medications, along with nonsurgical and surgical interventions. First-degree burns can be treated by immersing the affected area in cool to cold water and providing analgesics for pain. Topical OTC burn cream or aloe vera gel can be used to promote healing and limit scarring. Second-degree burns can be rinsed with cool water until the pain stops (10 to 30 minutes), and then additional cool compresses can be applied as needed. It is important to leave blisters intact. If a blister breaks open, the area should be bandaged to prevent infection. Elevating the limb can help to reduce the swelling. The same OTC creams suggested for first-degree burns can be used for second-degree burns. Both first- and second-degree burns can be treated at home, but the patient should seek medical attention if the area looks infected or is not healing. Third- and fourth-degree burns need immediate and ongoing medical attention. The area should be covered with sterile gauze or a clean cloth until medical intervention is obtained. Clothing stuck to the burned area should not be removed except by medical personnel. Pain medications may be prescribed, including analgesics or opioids. Antibiotics also will likely be prescribed. Third- and fourth-degree burns will often require skin grafts to close the wound. Treatment for these burns is an ongoing process.
Mohs Surgery
Mohs surgery is done to remove skin cancer lesions. The procedure involves repeated removal and microscopic examination of the layers of a lesion until no cancerous cells are seen (FIGURE 17.22). As with any surgical procedure, sterile technique must be maintained.
Psoralen Plus Ultraviolet A (PUVA) Therapy
A psoralen topical medication plus ultraviolet A (PUVA) therapy is used to treat a number of different skin diseases and is commonly used for psoriasis. The psoralen lotion or gel is applied to the affected area for 10 minutes to treat small areas before exposure to UVA.
Appearance Modification Procedures
The medical assistant may also provide help in procedures that can modify a patient’s appearance.
Chemical Peel (Chemoexfoliation)
Topical agents are used in chemical peels to minimize or remove minor skin features, such as acne scars, hyperpigmentation, and fine wrinkles. Agents used for chemical peels include tretinoin cream with 0.05% to 0.1% concentration (Retin-A) and a number of different acidic preparations. During application, care must be taken to prevent the solution from entering the eyes. The use of chemical exfoliating agents may cause the skin to appear inflamed and dry, with crusting and edema. The patient may complain of stinging and burning at the beginning of the treatment regimen. The patient should avoid sun exposure for the length of treatment and should use a sunscreen with a minimum SPF of 15 because photophobia (light sensitivity) is a typical side effect of treatment.
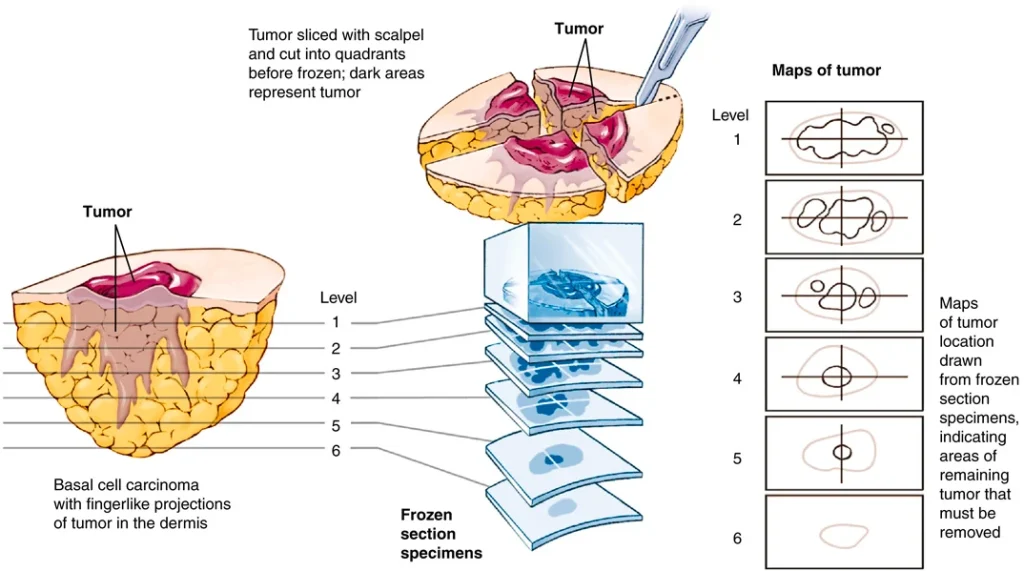
FIGURE 17.22 Mohs surgery. From Shiland B: Mastering healthcare terminology, ed 5, St. Louis, 2016, Elsevier.
Dermabrasion
A dermabrader is a handheld device that mechanically evens the layers of dermal tissue. It is effective in the treatment of scars from acne vulgaris. Topical anesthetics (e.g., ethyl chloride) or locally injected anesthetics are used for the procedure. Besides the dermabrader, the dermatologist may use a variety of wire brushes, abrasive discs, or other devices to smooth scar tissue. Standard Precautions must be followed, including the use of face and eye guards, to prevent aerosol or splatter contamination from the site. The patient should be educated about wound care, signs of infection, and the presence of photophobia for 6 to 12 months after the procedure.
Laser Resurfacing (Photothermolysis)
Laser therapy may be used to address fine lines and wrinkles, pigmented areas, shallow scars, and tattoo removal. Typically, the patient is instructed to prepare the site 3 to 6 weeks before the procedure with tretinoin (Retin-A), alpha-hydroxy solutions, or bleaches. Laser procedures are performed with the patient under local, regional, or general anesthesia. During the procedure, it is extremely important the patient and all personnel wear the type of eye protection recommended by the laser manufacturer. After the procedure, cool packs are applied to help reduce swelling, and topical antibiotic ointment is used to prevent infection. The treated area appears inflamed and edematous and can take up to 2 weeks to heal; it can take as long as 6 months for the inflammation to fade.
Botox Injections
Botox is a strong neurotoxin (a substance toxic to nerves) produced by Clostridium botulinum, a bacterium that causes food poisoning. Two strains of the botulism bacterium are used in dermatologic procedures for appearance modification. Botox treatments involve injection of the substance around the eyes, mouth, and forehead. The toxin interferes with nerve stimulation, which temporarily paralyzes the muscles of the face that cause wrinkles to form. It also smooths out the skin and makes it look younger and fresher. The effects are short term, so treatments must be repeated every 3 to 4 months, and some patients complain of an inability to show facial expression because of muscle paralysis.
